INTRODUCTION
Gene therapy products allow administration of nucleic acids to modify the genetic material of cells. Gene therapy products can be broadly classified based on the approach to delivery and include the following: (1) viral vectors [viruses that harbor the gene(s) of interest but usually without the mechanism to self-replicate in vivo]; (2) nucleic acids in a simple formulation (naked DNA); and (3) nucleic acids formulated with agents such as liposomes that enhance their ability to penetrate the cell. Where introduction of nucleic acid to cells takes place ex vivo, the cell population that is administered becomes the gene therapy product. Guidance specific to the manufacturing, processing, characterization, and administration of cell-based products is provided in Cellular and Tissue-Based Products  1046
1046 .
.
Decisions regarding the choice of a gene vector can be complex (see Design Considerations for Gene Vectors under Manufacturing of Gene Therapy Products). The viruses most commonly used include murine retroviruses, human adenoviruses, and human adeno-associated viruses (AAVs). It is inherent in the definition of gene therapy in this chapter that the administration of nucleic acid through transduction is expressed as RNA and then as protein. Examples of gene therapy products are shown in Table 1.
Table 1. Examples of Gene Therapy Products
| Categories or Strategies | Indication: Administered Product |
|---|---|
| Gene replacement Short-term Long-term |
Cardiovascular disease: growth factor vector on a biocompatible scaffolda
Cystic fibrosis: transmembrane conductance regulatory vector Hemophilia: factor VIII or IX vector |
| Direct cell killing | Cancer: recombinant oncolytic viruses |
| Immunotherapy | Cancer: autologous tumor cells transduced with cytokine or other immunomodulatory genes; lymphocytes transduced with receptors for tumor antigens Arthritis: gene-modified autologous lymphocytes |
| Conditionally lethal genesb | Cancer (solid tumor): thymidine kinase (TK) or cytosine deaminase (CD) vector into tumor cells Graft-versus-host disease (GVHD): TK or CD vector transduced into donor T cells |
| Gene disruption via antisense RNAs, ribozymes, and inhibitory RNAs expressed via a vector | Cancer: anti-oncogene vector Cytomegalovirus retinitis: anti-viral vector Human immunodeficiency virus (HIV): autologous lymphocytes transduced with antiviral ribozyme vector |
| Intrabodies | Cancer or HIV: vector encoding single-chain antibody to a tumor protein or a viral protein, respectively |
|
a
This product promotes formation of new blood vessels.
b
Cells with conditionally lethal genes as well as their neighboring cells are killed after the administration of a second drug in vivo. For TK, the drug is gancyclovir. For CD, the drug is 5-fluorocytosine.
|
|
Chapter Purpose and Organization
Clinical uses for gene therapy products, their manufacturing processes, and analytical schemes for determining identity, dose, potency, purity, and safety are rapidly evolving, and are as diverse as the products themselves. This chapter summarizes the issues and best current practices in the manufacturing, testing, and administration of gene therapy products. Usually USP chapters focus on materials that are commercially available. This chapter, however, not only discusses products for commercial applications, but it also addresses the production of clinical trial materials. When different approaches are options for clinical trial material compared to those used for commercial product, this is discussed.
Where appropriate, reference is made to applicable guidance including International Conference on Harmonization (ICH) quality guidelines because the principles apply even though gene therapy products may be outside the official scope. A list of regulatory and guidance documents applicable to gene therapy is presented in the Appendix, together with a list of terms commonly used in the gene therapy field. The traditional compendial perspective is to develop public standards that can be applied to a particular final product without providing production details. This chapter attempts to specify when traditional methodologies or standards can be adapted.
This chapter is extensive because of the diverse nature of the products and the special considerations that they require. Manufacturing has been divided into two sections: the first discusses general aspects of manufacturing and process development, and the second discusses vector design and class-specific topics. On-Site Preparation and Administration follows the manufacturing sections because the handling of these products at the clinic often requires facilities and expertise not found in a typical hospital. Other manufacturing-related sections include: Analytical Methods; Stability; Storage and Shipping; and Labeling. The section Regulations and Standards summarizes existing guidelines and highlights the need for the development and validation of new methodologies to assess product quality. The Glossary of Terms lists and defines the terms and abbreviations used in this chapter and those commonly employed in this field.
MANUFACTURING OVERVIEW
Introduction
The manufacturing of gene therapy products has been divided into two sections. This section, Manufacturing Overview, discusses five topics that apply to manufacturing of all gene therapy products: (1) raw materials, (2) characterization of banked materials, (3) in-process controls, (4) specifications, and (5) validation considerations. The second section, Manufacturing of Gene Therapy Products, addresses manufacturing of gene therapy vectors, both viral and nonviral, and discusses the design of gene vectors in detail.
All the general principles of current good manufacturing practice (cGMP) outlined by FDA in 21 CFR 210, 211, 600s (especially 21 CFR 610), and 820, as well as other USP chapters apply to the manufacturing of gene therapy products. The manufacturing facility, equipment and process, raw materials, quality systems, and trained personnel are some of the key elements of cGMP. cGMPs are applied throughout clinical development. Typically, the extent of control increases as clinical development progresses, and full cGMP compliance is expected by initiation of manufacturing in support of Phase III clinical trial(s). The facility and equipment should be carefully designed, built, and validated to support the manufacturing process and to maintain the required product/facility segregation. Preventive maintenance and calibration should be performed routinely on critical equipment. Incubators, bioreactors, and freezers should be fitted with alarm systems that can remotely signal failure. Quality systems should be established to ensure manufacturing is consistent and in control. Systems include but are not limited to the following: change control, document control, environmental monitoring, training, validation master plans, raw material testing and release, vendor approval, product testing and release, stability testing, and corrective/preventive action (CAPA).
Ancillary Materials
A wide variety of raw materials, including ancillary materials, may be used in manufacturing. Raw materials may include complex substances such as cells, tissues, biological fluids, growth factors, and monoclonal antibodies. Some of these materials may remain in the final therapeutic product as active substances, cryoprotectants, or excipients. An ancillary material exerts an effect on a therapeutic material (for example, a cytokine may activate a population of cells) but is not intended to be present in the final therapeutic product. The quality of raw materials used in the production of a gene therapy product can affect the safety, potency, and purity of the product. Therefore, qualification of this type of materials is necessary to ensure the consistency and quality of all gene therapy products. Activities involved with raw material qualification will change as products move through various stages of clinical development and on to licensure and commercialization. A well-designed qualification program becomes more comprehensive as product development progresses. A qualification program for raw materials used in the manufacturing of gene therapy products should address each of the following areas: (1) identification and selection, (2) suitability for use, (3) characterization, (4) animal-derived components, and (5) quality assurance. For all raw materials, it must be considered when and where each is used in the manufacturing process because this can help define selection criteria. USP chapter Ancillary Materials for Cell, Gene, and Tissue-Engineered Products  1043
1043 should be consulted for specific information about implementing an appropriate qualification program for these materials. Other USP chapters provide information about the qualification and standards of specific ancillary materials (e.g., Bovine Serum
should be consulted for specific information about implementing an appropriate qualification program for these materials. Other USP chapters provide information about the qualification and standards of specific ancillary materials (e.g., Bovine Serum  1024
1024 , Fetal Bovine Serum—Quality Attributes and Functionality Tests
, Fetal Bovine Serum—Quality Attributes and Functionality Tests  90
90 , and Growth Factors and Cytokines Used in Cell Therapy Manufacturing
, and Growth Factors and Cytokines Used in Cell Therapy Manufacturing  92
92 ).
).
Characterization of Cell and Virus Banks
cell banks
A cell bank is a collection of vials containing cells stored under defined conditions, with uniform composition, and obtained from pooled cells derived from a single cell clone. The cell bank system usually consists of a master cell bank (MCB) and a working cell bank (WCB), although more tiers are possible. The MCB is manufactured in accordance with cGMP and preferably is obtained from a qualified repository source (source free from adventitious agents) with known and documented history. The WCB is produced or derived by expanding one or more vials of the MCB. The WCB, or MCB in early trials, becomes the source of cells for every batch produced for human use. Cell bank systems contribute greatly to consistency of production of clinical or licensed product batches because the starting cell material is always the same. Cell banks used for the preparation of virus banks or clinical product should be suitably characterized before use. Aspects of cell banking and validation are addressed in Cellular and Tissue-Based Products  1046
1046 , Quality of Biotechnological Products: Analysis of the Expression Construct in Cells Used for Production of rDNA-Derived Protein Products
, Quality of Biotechnological Products: Analysis of the Expression Construct in Cells Used for Production of rDNA-Derived Protein Products  1048
1048 , and Viral Safety Evaluation of Biotechnology Products Derived from Cell Lines of Human or Animal Origin
, and Viral Safety Evaluation of Biotechnology Products Derived from Cell Lines of Human or Animal Origin  1050
1050 .
.
Virus Banks
The master virus bank (MVB) is similar in concept to the MCB because it is derived from a single production run and is uniform in composition. The working virus bank (WVB) is derived directly from the MVB. As with the cell banks, the purpose of a virus bank is to have a consistent source of virus that is shown to be free of adventitious agents for use in production of clinical or product batches. In keeping with cGMP regulations, testing of the cell bank that will be used for production of the virus banks, including quality assurance testing, should be completed before the use of this cell bank for production of virus banks.
Qualification
Cell and viral bank characterization is an important step toward obtaining a uniform final product with lot-to-lot consistency and freedom from adventitious agents. Testing to qualify the MCB or MVB is performed once, and can be done on an aliquot of the banked material or on cell cultures derived from the cell bank. Specifications for qualification of the MCB or MVB should be established. It is important to document the MCB and MVB history, the methods and reagents used to produce the bank, and the storage conditions. All the raw materials required for production of the banks—media, sera, trypsin, and similar substances—must also be tested for adventitious agents.
Qualifying the Master Cell Bank
The FDA Guidance for Industry: Human Somatic Cell Therapy and Gene Therapy (March 1998) provides specific recommendations for qualifying MCBs. Additional guidance is provided in ICH Q5D. A description and history of the cell line is required, along with a description of the freezing process, storage conditions, and the number of vials prepared. The identity of the cells should be analyzed by genotypic and/or phenotypic markers. For MCB containing vector sequences, the presence and integrity of the vector should be demonstrated using molecular assays (restriction endonuclease mapping and/or nucleic acid sequencing) and/or measurement of vector gene expression. Purity must be analyzed to exclude bacterial, mycoplasma, fungal, and viral contamination (other than vector sequences). Freedom from adventitious viruses should be demonstrated using both in vitro and in vivo virus tests and appropriate species-specific tests such as the mouse antibody production (MAP) test. Special attention should be given to the detection of replication-competent virus (RCV) arising from recombination of the vector and viral sequences. The MCB is further qualified by tests conducted on cells (from the MCB or WCB) expanded to the limit of in vitro cell age for production.
Qualifying the Master Virus Bank
Testing of the MVB is similar to that of the MCB and should include testing for freedom from adventitious agents in general (such as bacteria, fungi, mycoplasma, or viruses) and for organisms specific to the production cell line, including RCV. Identity testing of the MVB should establish the properties of the virus and the stability of these properties during manufacture.
Qualifying the Working Cell or Virus Bank
Characterization of the WCB or WVB is generally less extensive and requires the following: (1) testing for freedom from adventitious agents that may have been introduced during generation of the WCB, (2) testing for RCV, if relevant, (3) routine identity tests to check for cell line cross-contamination, and (4) demonstration that aliquots can consistently be used for final product production. This assumes that the WCB and WVB were prepared in a controlled environment using media and equipment that were screened appropriately for adventitious agents. If not, additional release testing is required.
In-Process Controls
Manufacturing processes should have well-defined go–no go decision criteria that are applied to key in-process intermediates and are used to pool material that has been processed through a step in several sublots. Quality must be built into the product as well as tested during batch release. In-process controls are the assays or tests that are performed to ensure that the in-process intermediate is of sufficient quality and quantity to ensure manufacture of a quality final product. Examples of in-process controls are listed in Table 2. The main reason for performing the in-process control is to ensure that the correct product with anticipated quality and yield is obtained. Intermediate in-process material that fails to satisfy the in-process control criteria should not be used for further manufacturing. This material may be reprocessed if there are procedures in place for such activities. The reprocessed material must satisfy the original in-process specifications before it can undergo further manufacturing. If several sublots will be pooled for further processing, sublots that fail to satisfy the criteria should not be included in the pool, even if the pool containing these failed sublots would pass the in-process assay criteria. During clinical development, assays for product quality and yield should be performed after most processing steps to determine which steps are critical and which assays are most sensitive to deviations in the process. The information from these runs is also used to set the criteria for the selected assays. In-process controls are performed for fully validated processes to ensure that the process continues to be under control. The results of these assays should be trended, and actions should be taken to correct problems as they arise.
Table 2. Examples of In-Process Control Applications
| Type of Product | Attribute to Control |
|---|---|
| Viral gene therapy | Quantity of virus after virus culture Specific activity of virus in fractions after column chromatography Quantity of host-cell DNA in fractions after column chromatography |
| Nonviral gene therapy | Optical density or change in oxygen consumption during culture Amount and form of plasmid before culture harvesting Amount and form of plasmid after extraction steps Amount of pyrogen or endotoxin after extraction steps in plasmid pool |
Specifications
The specification for a gene therapy product should be chosen to ensure the safety and efficacy of the product before use. Selected tests should be product specific and should have appropriate acceptance criteria to ensure that the product exhibits consistent quality parameters within acceptable levels of biological variation, loss of activity, physicochemical changes, or degradation throughout the product's shelf life. The development and setting of specifications for cell and gene products should follow the principles outlined in ICH Q6B and should reflect the FDA Guidance for FDA Reviewers and Sponsors: Content and Review of Chemistry, Manufacturing, and Control (CMC) Information for Human Gene Therapy Investigational New Drug Applications (INDs).
Establishing specifications for a drug substance and drug product is part of an overall manufacturing control strategy that includes control of raw materials, excipients, and cell and virus banks; in-process testing; process evaluation and validation; stability testing; and testing for consistency of lots. When combined, these elements provide assurance that the process is in control and that the key quality attributes of the product are maintained. Appropriate specifications are established on the basis of thorough characterization of the product during the development phase and an understanding of the process and its capability. Characterization should include measurements of the physicochemical properties, safety, purity, process and product-related impurities, potency, viability, sterility, and quantity. Specifications for each product and its ingredients should be developed from this information by application of appropriate statistical methods. The data should include lots used in preclinical and clinical studies and should also include assay and process validation data that can be correlated to safety and efficacy assessments. Specifications should accommodate the inherent variabilities exhibited by the production process and by the assay. Some lot-release specifications typically applied to biologics may require re-examination for these product types.
The procedures in a specification for the product are anchored by appropriate reference standards. The reference standard for the product ensures that the product, as measured by the release assays, does not change significantly over time. The reference standard is manufactured using the same process as used for clinical production and is subject to all in-process and final release testing. In addition, the reference standard may be subjected to additional characterization not typically performed as part of lot release. The reference standard need not be stored at the same dose, formulation, or temperature as the product, but the stability of this reference standard should be determined. The reference standard verifies that a test produces acceptable results (passes its system suitability tests). A specific assay standard (working standard) can be used in the test, but it should be calibrated against and behave like the reference standard. Changing to a new reference standard (lot) should include many tests, all of which are run side by side with the existing reference standard. The impact of any change in the properties of the new reference standard should be carefully evaluated before it is adopted.
Additional specifications may be needed to produce a safe and effective gene therapy product. These might relate to some of the controls and action limits used to maintain standards and consistency for raw materials, excipients, and the manufacturing process (see Ancillary Materials and In-Process Controls). Specifications should be established to allow acceptance of raw materials and excipients used in the final formulation of the product. In addition, tests should be performed at critical decision steps during manufacture or at points where data serve to confirm consistency of the process. In-process release specifications should be established for each control step. Heterogeneity can result from the manufacturing process or storage of the product. Therefore, the manufacturer should define the pattern of heterogeneity within the product and should establish limits that will maintain the therapeutic efficacy and safety of the product.
In some cases, specifications may be established for lot release as well as for shelf life. As discussed in ICH Q5C and Quality of Biotechnological Products: Stability Testing of Biotechnological/Biological Products  1049
1049 , the use of different specifications should be supported by sufficient data to demonstrate that the clinical performance is not affected. Acceptance criteria should be established and justified on the basis of data obtained from lots used in preclinical and clinical studies and lots used for demonstration of manufacturing consistency and on the basis of relevant development data such as those arising from validated analytical procedures and stability studies. Acceptance criteria should also be correlated with safety and efficacy assessments.
, the use of different specifications should be supported by sufficient data to demonstrate that the clinical performance is not affected. Acceptance criteria should be established and justified on the basis of data obtained from lots used in preclinical and clinical studies and lots used for demonstration of manufacturing consistency and on the basis of relevant development data such as those arising from validated analytical procedures and stability studies. Acceptance criteria should also be correlated with safety and efficacy assessments.
Once specifications have been established, test results should be trended. Results that are out of specification (OOS)—or even those that are out of trend—should be investigated before the material is considered for further processing. The purpose of an investigation is to determine the cause of the discordant result. FDA's Guidance for Industry: Investigating Out-of-Specification (OOS) Test Results for Pharmaceutical Production provides a systematic approach for conducting an investigation. An assay result can be rejected if it can be confirmed that an error, such as analyst error, calculation error, or equipment failure, has taken place. If the investigation concludes that the product is not within the specification, the lot should be rejected. In unique situations, a product that does not meet all specifications may have to be administered to a patient. However, procedures must be in place to govern the communication of the OOS results to the physician or to the person responsible for making the decision to use the product and to provide instruction for any follow-up testing, patient monitoring, and communication of those results.
Considerations for Validation
The potential for wide biological variation in gene therapy products, particularly for patient-specific treatments, affects the validation effort. Nevertheless, the basic principles of process validation for any biological product, including recommendations by ICH, FDA guidance documents, Validation of Compendial Procedures  1225
1225 , and Validation of Microbial Recovery from Pharmacopeial Articles
, and Validation of Microbial Recovery from Pharmacopeial Articles  1227
1227 , apply to the validation of most gene therapy products. Guidelines for validating viral vaccines can be relevant to gene therapy processes that produce viral vectors. The hold steps in a manufacturing process should be validated to ensure that in-process intermediates are within specification and that the quality attributes of the final product are maintained. Product-release assays should be validated before production of the materials for Phase III pivotal clinical trials.
, apply to the validation of most gene therapy products. Guidelines for validating viral vaccines can be relevant to gene therapy processes that produce viral vectors. The hold steps in a manufacturing process should be validated to ensure that in-process intermediates are within specification and that the quality attributes of the final product are maintained. Product-release assays should be validated before production of the materials for Phase III pivotal clinical trials.
Process validation demonstrates that the unit operations of the manufacturing process perform consistently and can generate a quality product that meets specifications. Because biological processes are prone to variability, the consistency and robustness of the manufacturing process should be determined by validating the process on at least three lots. Process validation issues pertinent to cell-based products are addressed in  1046
1046 .
.
If possible, the process should be validated for virus clearance according to principles discussed in ICH Q5A. If this is difficult because of the nature of the gene therapy vector (e.g., enveloped virus), additional characterization of cells and animal-derived components used in the production process should be considered. If the gene therapy product is manufactured in a multiproduct facility, validate cleaning of multiproduct equipment and rooms to demonstrate the effectiveness of cleaning agents to inactivate or remove virus.
MANUFACTURING OF GENE THERAPY PRODUCTS
Introduction
Principles for the production of pharmaceutical or biological products are also relevant to the production of gene therapy vectors for use in humans. The same cGMP requirements are applied to ensure that a high-quality product is delivered to the patient. Because of the nature of gene therapy manufacturing systems, most manufacturers face development issues such as scalability, yield, cost efficiency, and product stability.
Most gene therapy vectors have been produced only in relatively small batches necessary to meet the needs of early clinical trials conducted in small numbers of patients. However, the promise of gene therapy in larger patient populations has led to progress in large-scale production and purification technology. This section focuses on designing vectors for gene therapy and choosing a suitable production technology.
Design Considerations for Gene Vectors
Types of Vectors
Table 3. Types of Gene Vectors
| Viral | Nonviral | |||||||
|---|---|---|---|---|---|---|---|---|
| Family | Retroviridae | Adenoviridae | Parvoviridae | Herpes- viridae |
Togaviridae | Poxviridae | ||
| Examples species | Murine Leukemia Virus | HIV | Adenovirus | AAV | Herpes Simplex Virus | Sindbis | Poxvirus (Vaccinia) | Plasmid derived |
| Vector Characteristics | ||||||||
| Insert size limit | 8 kb | 8 kb | 4.3–34 kb | 4–5 kb | 40–150 kb | 5 kb | 25–50 kb | 12 kb |
| Chromosome integration | Yes | Yes | No, episomal |
Can be integrated or episomal | Can be integrated or episomal | No | No | Yes, but at very low frequency |
| Therapeutic expression | Stable | Stable | Stable or transient | Stable | Stable or transient | Transient | Transient | Stable or transient |
| Vector localization | Nucleus | Nucleus | Nucleus | Nucleus | Nucleus | Cytoplasm | Cytoplasm | Nucleus |
| Types of cells transduced | Dividing only | Dividing and quiescent |
Dividing and quiescent |
Dividing and quiescent |
Dividing and quiescent |
Dividing and quiescent |
Dividing and quiescent |
Dividing and quiescent |
| Efficiency of gene transfer | High | High | High | High | High | High | High | Low |
| Expression of viral proteins | No | No | Yes, unless viral genes deleted | No | Yes | Yes | Yes | No |
| Other | Tropism can be altered by pseudotyping | Can be used as a plasmid therapy system | ||||||
A typical gene therapy vector is composed of the following: (1) the vector backbone; (2) a promoter; (3) the therapeutic gene, either as cDNA or genomic sequence; and (4) a polyadenylation signal. A wide array of viruses—including murine and human retroviruses, adenoviruses, parvoviruses such as AAV, herpes viruses, poxviruses, toga viruses, and nonviral plasmid therapy systems—have been developed for gene therapy applications. These vectors (see Table 3) differ greatly in terms of their capacity to deliver genetic material and the duration of expression. Some viral vectors preferentially target dividing cells, but others are capable of transducing both dividing and nondividing cells. There are significant variations in transgene capacity (i.e., there are limitations on the size of the foreign DNA fragment that can be incorporated into the vector genome). The level, timing, and duration of gene expression required for a gene therapy product depends on the clinical indication. Low-level, long-term gene expression may be required for some diseases, including adenosine deaminase (ADA) deficiency or type A and type B hemophilia. High-level, short-term expression may be more appropriate for cancer when genes that induce apoptosis are used or for cardiovascular disease when preventing hyperproliferation of smooth-muscle cells that may impede restenosis of saphenous vein grafts.
Vector Design Criteria
Many types of gene therapy vectors are being developed, and the vector selected for a particular clinical application depends on the disease state, the target cell, and the intended route of administration. As shown in Table 3, capacity depends on vector type, so clinical applications that require a large amount of genetic material will limit the choice of vector system. The payload of a vector system becomes increasingly important when one designs vectors with genomic DNA or a vector that contains extensive regulatory sequences.
Vectors are also selected based on the intended duration of expression and the target cell. For example, retroviral vectors integrate stably into target cells and are therefore well suited for stem cells or lymphocytes that are expected to undergo extensive cell division. In contrast, adenoviral and plasmid vectors are episomal and may be lost during cell division. However, adenoviral vectors are attractive for vaccine development and cancer applications where tumor cell elimination is the goal. Other vectors, such as AAV, do not integrate at high efficiency but can be expressed long-term in nondividing cells such as neurons or hepatocytes.
Target cell type can also play into the selection of an appropriate vector system (see Targeting Transduction). For example, the adenoviral Coxsackie virus B and adenovirus receptor (CAR) is expressed poorly on hematopoietic tissues, which limits the usefulness of the vector system for blood-derived cells. Vectors based on murine retroviruses require cell cycling and are not well suited to the transduction of nondividing cells such as neurons.
The immune system can target both the viral components of the vector and the expressed transgene. Pre-existing antibodies or cellular immunity to certain vector systems can exist and may limit their usefulness. Vectors can elicit an innate immune response that can decrease the efficiency of gene transfer and may also induce a severe adverse event. A large number of current gene therapy approaches seek to limit toxicity and immune response by administration of vector to cells ex vivo. Nevertheless, the majority of diseases suitable for gene therapy will require in vivo administration, and ongoing research seeks vectors with limited immune recognition.
The route of administration and manipulation of the total dose of vector are strategies that can be used to compensate for some limitations of specific vector systems. Additionally, there are advantages and disadvantages for the manufacture of each of the different vector systems that should be considered when planning a clinical application. Production consistency favors systems with well-defined fermentation or culture systems, such as plasmid, retroviral, or adenoviral vectors. For viral vector systems that require helper functions (see below), a rationally engineered cell line can overcome the scalability and consistency limitations of co-transfections. Use of a cell line that is adapted to suspension culture can affect scalability and cost efficiency.
Targeting Transduction
To be effective, a vector must first find and transduce its target cell. Viruses have a natural host range that is strongly influenced by the expression of specific cell-surface receptors, the current phase of the cell cycle, and the route of administration. Integrins are a class of cell-adhesion receptors that interact with either the penton base or the fiber protein of adenoviruses. The fiber and penton base proteins of adenoviruses mediate binding to the CAR, CD46, and integrins. Adeno-associated viruses primarily interact with heparan sulfate proteoglycan and sialic acid receptors on the cell surface. However, interaction with secondary receptors such as integrins, laminin, and growth factor receptors is required for efficient cell entry and trafficking of virus particles to the nucleus. An amphotropic variant of the murine leukemia virus (MLV), commonly used for gene therapy applications, utilizes the sodium-dependent phosphate transporter RAM-1 to enter cellular targets. Expression levels of each of these receptors vary according to tissue type, which dictates the transduction efficiency of the vector.
The host and tissue range can be modified or targeted by biochemical and genetic manipulation of the vector. Alterations in the tissue and cell specificity of retroviruses—and lentiviruses in particular—occur largely though genetic pseudotyping. During this process, the envelope proteins that dictate virus binding and entry via a specific cellular receptor of one virus are replaced with the envelope protein of another retrovirus or with a protein from an entirely different virus such as the vesicular stomatitis virus glycoprotein. The relative complexity of adenovirus and adeno-associated virus capsids allows them to be genetically modified in several ways. Substitution of a single virus protein (e.g., adenovirus fiber or AAV VP1) with that of another serotype within the same family is very much like the pseudotyping process for retroviruses. However, mosaic virus particles created by interspersing individual capsid proteins from several different virus serotypes in one virion, and chimeric particles created by capsid proteins of two distinctly different serotypes on a particle of yet another serotype (e.g., adenovirus 35 knob on adenovirus 41 fiber on an adenovirus 5 particle) can also effectively change the types of cells and tissues that a vector can transduce. Although this approach may seem straightforward, certain modifications of virus capsid proteins at the genetic level do not facilitate virus particle formation. Although most modifications improve virus uptake in one specific cellular target, they may also increase uptake in several other tissues in which gene transfer would not be desirable. Thus, selection of proteins and ligands must be carefully considered and tested in preclinical models of disease before these vectors can be used extensively.
Viral coat proteins and nonviral vectors can be chemically modified for ligand-mediated receptor targeting. They can be conjugated to cell-targeting ligands by antibody–virus interactions with bi-specific antibodies. Molecular bridges like biotin–avidin complexes and chemical crosslinkers such as bifunctional polyethylene glycol (PEG) tethered to cell specific receptor-binding proteins are easily conjugated to virus particles and often are incorporated in targeting strategies. These approaches can easily be combined and/or exchanged with genetic modifications and with each other to create vectors that effectively target several receptors. Although the biochemical approach avoids the functional complications of introducing foreign domains into viral proteins, each lot of vector must be modified because progeny virus will default to their original genetically encoded tropism. Biochemical processes also require the use of multiple reagents, which may complicate transfer to the clinic.
Another common and effective strategy to target viral vectors to tumor cells takes advantage of the virus replication cycle. Deletion of genes critical for taking over functional cellular checkpoints to support normal virus replication allows the virus to replicate only in cancerous cells where those checkpoints are either defective or inactive. This effect can be further enhanced creating small mutations in virus replication genes driven by tumor- and tissue-specific promoters. With respect to cell cycling, adenoviruses and adeno-associated viruses easily infect both quiescent and dividing cells, but MLV-based retroviral vectors are efficient only when transducing rapidly dividing cells. Lentiviral vectors can infect quiescent cells, including cells of neuronal origin. In general, nonviral vectors can enter both dividing and nondividing cells but have lower transduction efficiencies than viral vectors. Transduction efficiencies of nonviral vectors can be enhanced by the formulation and direct injection in the tissue of interest.
Influence of Humoral Immune System and Complement
One of the most significant barriers to effective gene transfer is the humoral immune response to the vector. Regardless of the route of administration, the intended target cell, and the dose, the vector is likely to encounter some component of the immune system. For viral vectors, the humoral immune system cannot readily distinguish between wild-type viral infections and recombinant viral vectors because the humoral response is directed against proteins in the viral envelope or capsid. Protein-containing formulations of nonviral vectors can also elicit a humoral immune response. Specific and cross-reacting humoral responses may pre-exist because of natural exposure to wild-type versions of viral vectors, or they may be elicited during dosing, and the antibody response may vary in its capacity to diminish gene transduction in individual patients. Because neutralizing capacity is frequently enhanced upon multiple dosing, repeated administration can also be problematic. Some of these issues may be remedied by the use of nonviral systems. However, the level of transduction efficiency of these vectors is not currently sufficient for many gene-transfer applications. Transduction efficiency of all vectors is also importantly compromised by the complement system. Many complement proteins have a natural affinity for virus capsid proteins. This interaction initiates release of cytokines and chemokines that facilitate rapid removal of vector from the systemic circulation. This affinity is often heightened (especially in the case of retroviruses) when nonhuman cellular proteins and culture components (e.g., fetal bovine serum) are incorporated into and/or coat the virus particle during large-scale production. Use of producer cell lines of human origin and serum-free culture conditions has decreased inactivation of vectors by complement.
Several strategies for mitigating and avoiding the humoral immune response and complement inactivation have been developed. Increasing the vector dose to compensate for the neutralizing activity of the antibodies and altering dosing regimens to coincide with periods of low antibody titer are logical choices, but possible toxicity associated with high doses of virus and the individual variability of the immune response are potential negative consequences of this approach. Alternatively, viral vectors can be engineered to evade the immune system. One approach involves increasing expression of specific viral genes that allow the virus to evade the host's humoral response. Recombinant viruses constructed from serotypes with limited exposure rates such as simian adenovirus 7 can avoid neutralization in those previously exposed to more common serotypes. Mosaic and chimeric viruses can also avoid neutralization. Both approaches effectively address the issue of efficient gene transfer in those with pre-existing immunity, but both approaches require further investigation in response to concerns regarding safety and large-scale production as well as induction of immune responses in naive patient populations. Covalent attachment of polyethylene glycol (PEGylation) to the virus capsid can both protect the virus from neutralization and blunt the immune response. Pharmaceutical methods such as embedding viral vectors in polymer matrices and administration of vectors to the mucosa (oral and nasal) can also protect viral vectors from the humoral immune response.
Influence of Cellular Immune Responses
Once transgene expression is initiated, cellular immune responses rapidly remove cells transduced by both viral and nonviral vectors. This decreases the overall therapeutic effectiveness of gene transfer of low-to-moderate vector doses and can be highly toxic when higher doses are administered. Active protein synthesis is not required for cellular immune responses to viral capsid proteins. For example, the capsid proteins of recombinant AAV vectors have been shown to be long-lived, leading to a delayed immune response and elimination of vector-transduced cells. De novo synthesis of viral gene products can also exacerbate host-cellular responses. Viral vectors have been designed with specific backbone deletions to eliminate the expression of viral structural genes and reduce this effect. Examples of such vectors include gutless adenoviruses, herpes viruses, and adeno-associated viruses in which all viral genes have been deleted, making them dependent on another helper virus for subsequent replication. Certain plasmid sequences, especially those with unmethylated CpG dinucleotides, can elicit a strong cellular immune response and have been used as adjuvants in some DNA-based vaccines. Amplifying plasmids in bacteria that express the CpG Methylase (M.SssI), removal of CpG sequences by site-directed mutagenesis, and removal of unnecessary prokaryotic sequences to create minimal plasmids have reduced the incidence of unwanted cellular responses. One nonmolecular approach to minimize the cellular response against the vector involves the use of immunosuppressants (cyclosporine, sirolimus, dacluzumab) at the time of initial vector administration as well as methods described for reducing the humoral response (use of chimeric vectors, PEGylation) outlined above.
Antigenicity of the Gene Therapy Product
In many cases, the gene therapy product and associated promoter and enhancer elements are antigenic in certain cellular targets. When proteins that are retained in the target cell are used, cellular responses may eliminate the target cell. If sustained protein expression is required, the cellular immune response may decrease the effectiveness of the therapy or eliminate it entirely. In terms of treating genetic diseases, patients with a null mutation who have never seen the transgene product may be at a higher risk for immune response than patients who produce a defective protein. Also, truncation of a gene such as the cystic fibrosis transmembrane conductance regulator (CFTR) so that it fits within a chosen vector may result in creation of a distinct antigen.
In other applications, the transgene product is a foreign protein, e.g., thymidine kinase derived from the herpes simplex virus (HSV), and thus may elicit an immune response. In some cases this is the desired therapeutic effect, particularly in antigen-based immunotherapy for cancer or a viral disease. Efforts to minimize the immune response against elements associated with the transgene cassette include designing vectors with the ability to carry full-length humanized sequences for the transgene of interest and administration of immunosuppressants at initial dosing and other intervals throughout the treatment protocol.
Vector Localization within the Target Cell
Once the vector reaches the target cell, several factors can affect the level and duration of therapeutic gene expression, and these factors dictate the choice of an appropriate vector system for a specific clinical indication. The localization of the vector genome within the cell, the strength of the gene expression control elements, the stability of the message, and the stability of the translated protein all affect therapeutic impact. Alphavirus-based vectors, such as those derived from Sindbis or Semliki Forest virus, reside in the cytoplasm and typically exhibit a very high level of gene expression. Retroviral, adenoviral, and other viral vectors have advantages in gene delivery with their natural mechanisms for nuclear delivery of the therapeutic gene and reasonable levels of gene expression from viral or other promoters. Nonviral plasmid vectors are episomal and are often susceptible to DNA degradation when they are shunted into cell endosomes. However, some nonviral systems incorporate nuclear targeting signals as a means of increasing therapeutic gene transcription efficiency.
Tissue-Specific Expression
Another means of controlling gene expression is the incorporation of tissue-specific promoters to stimulate or to restrict expression of the therapeutic gene. Unfortunately, many tissue-specific promoters do not provide high levels of gene expression, and incorporating these sequences into viral vectors may result in loss of specificity or low-level expression in cells that do not normally express the promoter. Tagging vector with sequences recognized by the microRNA system has also permitted tissue-specific expression and may offer tighter control than typically seen with tissue-specific promoter systems.
Drug-responsive promoters are being used to control gene expression. Rapamycin, mifepristone, and tetracycline (tet-on) systems have been used to repress gene expression. This type of regulation is particularly useful when constitutive expression of the vector transgene is toxic.
Impact of Replication Status of Vector
Replication status is another important consideration for vector design and selection. Viral vectors are most frequently constructed to be incompetent or replication-defective in order to limit uncontrolled vector spread and pathogenicity. However, the ability to replicate and spread within a specific cell population, e.g., within a tumor or to metastatic sites, may provide a significant therapeutic advantage over cell-type–specific targeting of replication-incompetent vectors. Replication can be engineered to be conditional when, for example, specific viral gene interactions are matched with intracellular pathway targets by means of targeted deletions and/or changes in transcriptional or translational control. When these targets are defective or missing, as in cancer cells, the virus can replicate, but when the target cell is functioning normally, viral replication is repressed. Viruses that have been genetically engineered for selective oncolytic replication include: adenovirus, HSV, vaccinia, measles virus, picornaviruses, influenza virus, Coxsackie virus, and Sendai virus. Some nongenetically-modified viruses are inherently oncolytic in human cells, e.g., reovirus and Newcastle disease virus.
One of the risks inherent in the use of conditionally replicating viral vectors is that such systems are leaky, i.e., the growth of the virus is not absolutely restricted to a single cell type. Also, subsequent rounds of viremia become considerations in the evaluation of tissue distribution/exposure and shedding. The therapeutic promise of these approaches depends on the reliability with which conditionality of replication can be selected or engineered. This therapeutic potential will be realized only if balanced with steps to control the potential risks to patients (associated with replication competence of the viruses/viral vectors) and to address associated shedding-related issues of third party exposure and environmental concerns.
As a proactive contribution to the safety profile and to take advantage of scientific and clinical information already available, virus strains that have been used for human vaccination are often used as the vector backbone. Nevertheless, because the product is replication competent, it presents specific technical challenges for adventitious agent testing and product characterization.
Nonviral vectors are normally designed as nonreplicating systems, but some groups are experimenting with replicating nonviral plasmids to increase gene expression levels (because of the low transduction efficiency of most nonviral systems) and to increase the duration of gene expression. Additional preclinical studies are needed to establish the safety of these systems. Artificial chromosomes have also been designed to take advantage of normal mechanisms for retaining gene expression in rapidly dividing target cells.
Vector Integration
The duration of gene expression is also a function of the persistence of the vector genome in target cells. Retroviral vectors can stably integrate into the host-cell genome, providing long-term expression. Adenoviruses and nonviral plasmid vectors, e.g., those not administered using electroporation, do not integrate, and expression generally decreases over time. Recombinant AAV vectors generally do not integrate, and when they do, it is not site specific. However, stable episomes have been observed in certain cell types such as muscle cells.
Site-specific integration can be a desirable feature for vectors that are intended to correct genetic disorders. Although it is not currently efficient enough to be useful, the control of the site of integration is desirable in order to prevent insertional mutagenesis. Insertional mutagenesis has the potential to kill a cell if a critically functioning gene is inactivated or to predispose a cell to malignant transformation if a tumor-suppressor gene is inactivated. Of clinical relevance, promoter or enhancer elements within vectors can lead to activation of cellular oncogenes and have been associated with malignant transformation in children undergoing retroviral gene transfer for X-linked severe combined immunodeficiency.
The success of any gene therapy product depends on the relationship between the vector-delivery system and the requirements of the disease in terms of the site, level, and duration of therapeutic gene expression. A universal vector now appears unlikely, and the challenge lies in fitting one of several possible vectors to the disease and to the gene to be delivered.
Manufacturing and Purification Strategies
Vector Construction
Viral and nonviral gene-transfer vectors are constructed by using standard molecular biology protocols. For viral vectors, the vector backbone consists of viral RNA or DNA sequences from which the regions encoding viral structural genes or the regions required for replication have been deleted. The deleted region of the vector is usually modified with specific restriction endonuclease sites used to allow insertion of the gene of interest. For nonviral vectors, the plasmid DNA backbone contains multiple restriction sites for cloning and the bacterial elements necessary for plasmid production. Vector backbones can accommodate single or multiple gene insertions depending on the maximum amount of sequence they can carry. The promoter that facilitates transcription of the gene insert can be a related viral promoter, such as the murine leukemia virus long terminal repeat (MuLV LTR), or a heterologous promoter that is either tissue specific, such as the alpha crystalline promoter (of the eye), or constitutive, such as the cytomegalovirus (CMV) late gene promoter. For example, in a retroviral vector construct containing two gene inserts, transcription of one is regulated from the 5¢-LTR-promoter sequence, and a second gene insert can be linked to an internal heterologous promoter from Simian virus 40 (SV40).
The complementary DNA (cDNA) containing the therapeutic gene of interest, including its introns, is excised from its source using restriction enzymes and is inserted at the multiple cloning site of the gene-transfer vector. The polyadenylation signal can be derived from multiple sources such as the SV40 virus or human growth hormone gene. Characterization and testing of gene therapy vectors are described under Analytical Methods.
Helper Function Systems
Recombinant viral vectors are most often modified to be replication defective, a condition created by deletion or modification of the viral genes needed for replication and production of infectious virus. Because the vectors are stripped of some or all of the viral genes, a system must be developed to supply viral proteins and to encapsulate the vector into a viral particle. Generally, this is accomplished by two methods: transient transfection or stable packaging cell lines.
In the transient transfection method, a series of different plasmids are generated, including a plasmid containing the vector and another vector containing the viral genes. For example, retroviral vectors can be generated using a three-plasmid system: (1) the transgene-containing vector plasmid; (2) a plasmid containing the gag/pol viral gene region; and (3) a plasmid containing the viral envelope. All three plasmids are transfected into cells, e.g., HEK293 or HT1080, and vector-containing virions are harvested after two to three days. The separation of vector and viral genes on different plasmids, along with vector designs that minimize the homology between vector and viral sequences, decrease the chance for recombination and generation of replication-competent virus. Similar approaches can be taken with most viral vector systems.
The transient transfection method has the advantage of a rapid production time and flexibility when changing components of the vector or viral constructs. Nevertheless, it can be cumbersome when scaling up for manufacturing, and special care must be taken to provide consistent production yields. An alternative method has been the use of vector packaging cell lines. In this scenario, the viral genes are introduced stably into an immortalized cell line that yields persistent expression of viral genes. As with transient transfection, the viral genes generally are expressed from different plasmids to decrease the risk of recombination. Since plasmids integrate infrequently, considerable time and effort are required to isolate a high-titer packaging cell line and to generate an MCB. Vector constructs can be introduced into cells from the MCB, and researchers, by screening for a high-titer clone may allow isolation of a stable cell line that generates the vector of interest. These cell lines generally can be expanded to great numbers and often produce vector for up to a week at a time, facilitating vector scale-up and product consistency.
Typical helper function systems are as follows:
Retroviral Vector Systems—
Initial packaging cells were based on the murine fibroblast cell line NIH 3T3. The PG13 cell line (expressing the Gibbon Ape Leukemia Virus envelope) has been used extensively with a low incidence of recombination events leading to RCV. More recently, the human HEK293 and HT1080 cell lines have been modified to serve as packaging cell lines for retroviruses. The use of a human cell line decreases elimination of vector particles by the human complement system (although this is generally not a concern for vectors used in ex vivo protocols).
Adenoviral Vector Systems—
HEK293 cells are widely used to supply the E1 function necessary for efficient adenoviral replication that is deleted from first-generation adenoviral vectors. Other complementing cell lines, such as E1-modified A549 cells (human lung carcinoma) and the PER.C6 cell line (human embryonic retinoblast), have also been created to supply E1 or other missing functions. PER.C6 contains the E1 region under the control of a phosphoglycerate kinase (PGK) promoter and has no flanking adenoviral sequences in order to eliminate production of replication-competent adenovirus (RCA).
AAV Vector Systems—
These systems classically use adenovirus-infected HEK293 cell lines transiently transfected with AAV helper plasmid containing the rep and cap genes, which are required for AAV replication and capsid formation, respectively, and are deleted from the AAV vector. In some AAV production systems, wild-type adenovirus has been removed from the process by using triple transfection of plasmids expressing Ad early genes, rep and cap, and the vector transgene. The HeLa cell line (from human uterine cervical carcinoma) has also been used as a transient production system. More recently, both of these cell lines have been used to establish stably transfected packaging cell lines that express rep and cap genes and in some cases express the adenoviral functions needed for AAV replication when rep and cap are present (E1a, E1b, E2a, E4, and VA RNA). AAV production systems using recombinant HSV and Baculovirus have also been developed.
Gutless Adenoviruses—
Early manufacturing systems for the adenovirus vector known as gutless adenovirus were similar to classical AAV vector manufacturing systems because HEK293 cells were transiently transfected with helper plasmid containing required adenoviral functions. Development of helper viruses housing a packaging signal flanked by loxP sites and complementing HEK293 cell lines that express the bacteriophage P1 site-specific Cre recombinase has greatly improved the yield of the gutless virus. This technology notably reduces the amount of helper virus contamination by preventing packaging of the helper virus genome while permitting it to replicate and support replication and encapsidation of the gutless vector.
Viral Gene Therapy Vectors
Retrovirus and adenovirus vectors typically have been produced at laboratory, non-GMP scale by use of traditional cultivation methods for anchorage- and serum-dependent cell lines employing flasks, trays, and roller bottles. Initially, gene therapy vectors were produced by these methods because large volumes of product were not required for early clinical studies. Cell-bank systems are used as the source of cells, and virus banks are the source of virus for clinical production. In many cases, supernatant is collected, clarified, and stored frozen in bags at  70
70 . In many early clinical trials, unpurified supernatant has been used for ex vivo gene transfer.
. In many early clinical trials, unpurified supernatant has been used for ex vivo gene transfer.
Larger-scale upstream production methods have been reported and are commonly used. They include suspension, bioreactor, and fixed-bed or microcarrier culture methods. Some groups have reported adapting their process cells to serum-free culture conditions. Cells are harvested and lysed or supernatant is collected. The harvest is clarified and purified to remove host-cell debris, host-cell DNA, and other process-derived contaminants.
Traditionally, viruses are purified by gradient ultracentrifugation, but this is time-consuming and unsuitable for larger-scale production purposes. The selection of downstream process steps and their sequence is determined by the nature of the virus itself and the upstream process used for manufacturing the virus. As processes are being developed for the manufacture of gene therapy vectors, many different purification steps have been reported. These include ion-exchange and sulfonated-cellulose chromatography, zinc ion affinity chromatography, and size-exclusion chromatography. Typically, DNase or other nuclease treatments are used in the process in order to reduce host-cell or plasmid DNA. AAV production and lentiviral production are complicated by a need for transient transfection or co-transfection of plasmid or helper virus. These processes have generally required anchorage-dependent cell lines that are difficult to scale up. The development of stably transfected cell lines would allow large-scale production.
Purification Methods: Viral Vectors
Retroviruses—
To date, purification of retrovirus preparations for phase I clinical trials has often been minimal at best, i.e., the simple concentration of culture supernatants is insufficient to meet the stringent quality standards required for in vivo therapy. Centrifugation and microfiltration techniques are very useful for clarification of culture supernatants and removal of cellular debris. Ion-exchange, size-exclusion, and affinity chromatography techniques have also been employed to remove excess salt, serum, and low molecular weight contaminants also concentrated with the virus.
Adenoviruses—
Recombinant adenoviral vectors were often purified by cesium chloride density gradient ultracentrifugation. This is still used for research-scale preparations, but the procedure is neither scalable nor efficient for large quantities of clinical-grade virus. The most recent scalable purification methods use anion-exchange chromatography because of the strong affinity of intact virus particles for the resin with respect to that of cellular and individual capsid proteins. Published loading estimates for anion-exchange resins range from 0.5 × 1012 to 5 × 1012 virus particles/mL of resin or 0.14 mg of virus to 1.4 mg of virus/mL resin. Gel filtration and immobilized metal affinity chromatography are often used in polishing steps following anion-exchange purification of recombinant adenovirus-based products.
Adeno-Associated Viruses—
The toxicity of cesium chloride, the aggregation of AAV particles, and the fact that adenovirus is not completely removed after extensive centrifugation complicate AAV purification by cesium chloride density gradient ultracentrifugation. Another density separation medium, iodixanol, which is less toxic than cesium chloride and prevents AAV aggregation, has been employed in a single centrifugation step. Passage of the AAV fraction over an affinity column consisting of either a heparinized support matrix or monoclonal antibodies produced against AAV2 strongly increased purity and infectivity of final preparations. These methods are appropriate only for specific AAV serotypes. Ion-exchange chromatography is the most powerful and versatile method for AAV purification, although buffer pH, detergent concentration, and column medium must be tailored for each AAV serotype. Infectivity and purity of preparations obtained from these purification strategies are comparable to those obtained from affinity chromatographic methods and are complete within three hours.
Plasmid or Nonviral Vectors
Plasmids are double-stranded, circular DNA molecules that exist in bacteria as extrachromosomal, self-replicating molecules. They have been modified to serve as cloning systems, to contain multiple restriction endonuclease recognition sites for insertion of the cloned transgene, and to contain selectable genetic markers for identification of cells that carry the recombinant vector. Plasmid-based, nonviral vectors are frequently used as gene delivery systems for both in vivo and ex vivo gene therapies. These vectors are in the form of naked DNA or are complexed with lipids or other agents that facilitate transfer across the cell membrane and delivery to the cell nucleus without degradation. An advantage of a plasmid-vector system is the efficient production of large quantities of the vector that is easily characterized and avoids the risk of RCV associated with many viral systems.
Nonviral vectors are typically produced by using an Escherichia coli bacterial system. Plasmids are transfected into E. coli, and an appropriate single bacterial colony is selected and expanded to create an MCB. After reselection of a colony from a bacterial plate inoculated from the MCB, plasmid DNA is isolated from cultures that can range in size from 1 L on a laboratory scale to hundreds of L in bacterial fermenters. Plasmid DNA can be purified by several methods including affinity or ion-exchange chromatography and cesium chloride–ethidium bromide density gradients. Cesium chloride–ethidium bromide density gradients are not recommended for production of clinical-grade material.
Production and Processing of Nonviral Vectors
One benefit of nonviral vectors for gene transfer is that the production process is rather generic and can be applied to any plasmid preparation regardless of composition or application. Because the current average human dose of plasmid DNA for gene transfer and vaccination is approximately 1 mg, the primary challenge associated with large-scale production of plasmids is to develop a process that is both scalable and economical. Thus, process development for plasmid-based vectors remains an active area of research and development. A standard process for large-scale production of recombinant DNA plasmids consists of the followinfg five unit operations.
Fermentation—
Fermentation processes must support growth of transformed bacteria and maximize the amount of plasmid produced by each cell. E. coli is the most common strain used for plasmid production. Amino acids, nucleosides, and the ratio of nitrogen to carbon-containing compounds present in a rich media formulation greatly improve plasmid yield.
Harvest—
Bacterial cells are harvested either by centrifugation or microfiltration. Centrifugation under GMP conditions can be costly, which makes microfiltration the accepted method of cell harvest. This also allows spent media, metabolic byproducts, extracellular debris, and impurities to be washed away before purification.
Lysis—
Bacterial cells must be lysed to release the recombinant plasmids. This is one of the most critical steps in the production process because it can significantly affect the amount of usable [covalently closed circular (ccc)] and unusable [sheared, partially denatured, and open circular (oc)] forms of DNA in a preparation. The most widely used method of lysis for clinical-scale manufacturing is treatment with alkaline detergent and precipitation of cellular debris with acetate. This removes a large fraction of cellular impurities from the lysate, but it also increases the sensitivity of plasmids to mixing and localized concentrations of detergent, which are hard to manipulate on a large scale. Lysis of cells by heat exposure addresses this issue and effectively denatures cellular proteins and bacterial DNA.
Isolation/Purification—
Some processes include additional steps for removal of cellular debris and other contaminants from crude bacterial lysates by precipitation with detergents, polyethylene glycol, or salt. These reagents affect plasmid stability and are removed by column chromatography. Size-exclusion chromatography can effectively separate plasmid DNA from RNA, proteins, and other small molecules present in the cleared lysate. The degree of separation of plasmid DNA from contaminants is highly dependent on the type and concentration of salt in the running buffer. Resins used in anion-exchange chromatography have a high affinity for plasmid DNA and provide maximal sample concentration. Hydrophobic interaction and thiophilic aromatic chromatography are the methods of choice for selective separation of the different plasmid DNA isoforms and endotoxin reduction.
Bulk Preparation—
After purification, the bulk plasmid is placed in a suitable buffer and formulation by ultrafiltration using a membrane with a pore size of 50–100 kDa.
Plasmids for clinical use must be highly characterized. Impurities from production and processing steps are well known. Tests necessary to confirm the identity, purity, and potency of a plasmid-based product are well established and routine. These tests and the current specifications set by FDA and the World Health Organization are summarized in Table 4.
Table 4
| Assay Type | Issue | Determined By | Acceptable Level in Final Product |
|---|---|---|---|
| Identity | Cross-contamination with other products | Restriction digest/gel electrophoresis | N/A |
| Purity | Residual bacterial chromosomal DNA | Real-time PCR | <2 µg/mg DNA |
| Residual RNA | Analytical HPLC | <0.2 µg/mg DNA | |
| Residual bacterial protein | BCA protein assay | <3 µg/mg DNA | |
| Endotoxin | LAL assay | <10 EU/mg DNA | |
| Sterility (bacterial and fungal) |
Method outlined in 21 CFR 610.12 | No growth | |
| Appearance | Visual inspection | Clear solution free of particulates |
|
| pH | pH meter | Physiologic (7.0–7.4) but may be product specific | |
| Plasmid confirmation (ccc vs oc) | HPLC or CGE | >97% ccc | |
| Potency | Labeled dose | In vitro ELISA FACS RT-PCR Light absorbance (A260) |
Transgene/plasmid specific |
Introduction of Genetic Material into Cells—Gene-Modified Cells
A common extension of cell therapy involves the introduction of genetic material, usually DNA, into cells to alter their pattern of gene expression. While discussion focuses on DNA, similar scenarios can be applied to RNA or a derivative of DNA, except that the stability and solubility of the particular nucleic acid may dictate modifications of certain steps. The general process is often referred to as ex vivo gene therapy because the cells are removed from the patient or donor and the genetic material is introduced while the cells are outside of the body. The genetically modified cells are then administered to the patient. The genetic material introduced can either cause expression of new genes and products or inhibit the expression of already expressed genes and products. The latter represents a type of antisense therapy. The genetic material can be introduced by the same range of reagents that are involved with gene therapy: viral vectors, nucleic acids in a simple formulation (naked DNA), or nucleic acids formulated with agents such as liposomes that enhance their ability to penetrate the cell. Most of the steps and considerations discussed above also apply to the ex vivo introduction of genetic material into cells. The main goal of ex vivo therapy is to develop robust processes that will work with the majority of the patient's or donor's cells. This takes considerably more effort than processes for cell lines.
The method for introducing new genetic material into cells depends on the biology of the system and the desired stability of gene expression. If a simple retroviral vector such as Molony murine leukemia virus is used for transduction, the cells must be actively dividing because vector DNA is integrated into the cellular DNA only during replication. This usually leads to long-lasting expression of the desired gene product. Adenoviral vectors, naked DNA, or formulated DNA can be introduced into nondividing cells. However, gene expression will be transient because the introduced DNA will usually be extrachromosomal.
The main challenge in ex vivo gene therapy is to achieve efficient transduction or transfection, introducing sufficient DNA into the cell before the DNA degrades. In the case of transduction by simple retroviral vectors, cells are stimulated with reagents that cycle them into the S phase (replication) at the time that the vector is applied. Most retroviral vectors are stable in cell culture for a period up to a few hours. Because diffusion is minimal, only a small fraction of viral particles will come into contact with cells during this period. The following techniques can be used to increase the number of viral particles that contact the cell in a given time period:
- Maximization of viral particle concentration and minimization of the media volume during the transduction step
- Multiple applications of the virus
- Centrifugation of virus particles onto the cells
- Placing cells on a filter and slow pulling viral media through the filter
- Addition of binding-enhancing polymers to the media. [Note—Co-culturing the target cells with the viral producer cells is not recommended. This technique increases the chance of a recombinant event and production of RCV. Furthermore, any product for which co-culturing is used to transduce the human cells would be considered a xenotransplant if the producer cells were not human. The second cell type, whether human or not, may cause inflammation. ]
Each of these techniques has its own set of issues that must be addressed in order to develop a robust process. In technique 1, reduction of the volume during transduction results in rapid exhaustion of the medium, so supplemental medium should be added within a few hours. In technique 2, the cells may no longer be in the correct cell cycle phase during later applications, or cells may have become refractory because of unproductive transformation during the previous application. Techniques 3 and 4 can work well on a very small scale, but the number of cells that can be transduced may be insufficient to obtain an efficacious dose. In technique 5, polymers may fail to provide a benefit because virus binding may involve specific receptors for which surface density may prove to be the limiting factor.
Similar issues and techniques can apply with other viruses or DNA preparations. The issue of slow diffusion is even more marked for the use of DNA preparations. Factors such as the cell type in which the viral vector was produced, the media used for vector production, and the purity of the vector can have a pronounced effect on the efficiency of transduction. Although certain methods may not require cells to be actively cycling, in practice, most processes require that cells be capable of replication because of the following considerations:
- Safety considerations may dictate that only cells that express the new DNA are returned to the patient, which requires that these cells be selected. As described below, the most common selection method uses an antibiotic-resistant gene that is co-introduced with the new genetic material.
- Further propagation may be required to achieve the therapeutic dose of cells.
- Economic, biological, or technical reasons may dictate that the DNA introduction step be carried out at a low cell number and that the desired cell population then be expanded to the required dose.
Therefore, conditions that enable the cell or maintain its ability to proliferate must be developed in almost all cases. The biology of the cells, the available technology, and process economics will determine whether cells are propagated before, after, or during the introduction of new genetic material. Most processes do in fact expand the population after the introduction of the new gene.
Whether cells that do not productively express the gene can be administered to patients depends on the biology of the application, the dose required versus the handling capability of the manufacturing system, and, most importantly, the toxicity of the nonproductive cell population. Selection of the genetically modified cell population is commonly carried out using an antibiotic-resistance marker gene, such as neomycin, which is co-introduced into the cell with the new genetic material. For neomycin selection, cells in culture are treated with the antibiotic G418 at a concentration and for a period that has been shown to kill cells with nonproductive expression while allowing the productively expressing cells to proliferate. In this manner cells that are resistant to the antibiotic are presumed also to express the DNA of interest. The expression should be tested as a lot-release requirement or verified in a series of mock runs. Because most antibiotics decrease cellular proliferation, optimization of the culture media composition may be necessary for efficient selection and propagation of the gene-modified cells.
Following the antibiotic selection step, a second phase of antibiotic-free cell propagation may be required in order to achieve the desired dose and to rinse residual G418 out of the system. The selected medium and the total time that the cells are in culture can be critical to maintaining the desired expression of the original differentiated functions. An additional issue associated with the use of selection markers is that they generally are nonhuman genes. The expression of these genes usually elicits an immune response. Process development is often carried out with cells from healthy donors. Consideration should be given to the fact that for very sick patients, healthy cells that can be stimulated to undergo efficient, sustained replication are difficult to obtain.
Manufacturing, cell processing, and analytical testing issues pertinent to cell-based products are addressed in chapter  1046
1046 .
.
Formulation of Gene Therapy Products
Final formulations for gene therapy products are still in early development, and currently most gene transfer vectors are stored in solution at ultra-low temperatures. Successful formulation of candidates for gene transfer relies on a thorough understanding of the physicochemical and biological characteristics unique to each vector system. Factors like solution pH, ionic strength, and osmolarity influence the thermal stability of viral and nonviral vectors. Organic carbohydrates such as mannitol, sorbitol, sucrose, and trehalose have been incorporated into preparations to prevent disruption of the native conformation of the vector in solution, during the freeze-thaw process, and during lyophilization. Amino acids such as arginine and leucine have been incorporated into formulations for their buffering effects and to prevent aggregation. Surfactants such as the Tweens, Spans, and Pluronics have been effective at preventing aggregation, but this effect is somewhat vector specific because some vector products are easily disrupted by these reagents. Lipids, polymer and extraneous proteins (human albumin and gelatin) have also been incorporated in many vector preparations because of their ability to prevent loss of vector from direct interaction with pharmaceutical surfaces and during freeze-thaw cycles.
Before initiating a program for formal screening of formulations for a vector, the following factors should be considered. The required dose and/or storage concentration of the final product, as well as the specifics of the container-closure and/or delivery system should be established. Analytical methods to assess potency and identify degradants should be in place. The expectations of the formulation must also be defined. Some pragmatic criteria for the design and selection of vaccine formulations for use worldwide are: (a) the final product should be in a formulation that affords an 18- to 36-month shelf life when stored at 2 –8
–8 or above, (b) the formulation should have an acceptable stability profile at ambient temperatures to cover short-term storage and transportation in the field, (c) it should adequately protect the vector from damage during freeze-thaw cycling, and (d) it should consist of reagents that are pharmaceutically acceptable and within physiologically acceptable concentrations. Formulation changes during clinical development must be supported with preclinical studies and stability data. Sufficient time should be built into plans to account for this.
or above, (b) the formulation should have an acceptable stability profile at ambient temperatures to cover short-term storage and transportation in the field, (c) it should adequately protect the vector from damage during freeze-thaw cycling, and (d) it should consist of reagents that are pharmaceutically acceptable and within physiologically acceptable concentrations. Formulation changes during clinical development must be supported with preclinical studies and stability data. Sufficient time should be built into plans to account for this.
To date, little work in the area of formulation development of retroviral vectors with additives approved for human use has been described. The most significant effort to develop stable formulations for gene transfer has been with recombinant adenoviruses. Recently, identification of the mechanisms by which recombinant adenoviruses degrade in solution led to the development of several liquid formulations that stabilize the virus for up to 18 months at 4 . Adeno-associated viruses are regarded as one of the most stable viral vectors. This virus has been documented to be stable for approximately 4 months in phosphate buffered saline at 4
. Adeno-associated viruses are regarded as one of the most stable viral vectors. This virus has been documented to be stable for approximately 4 months in phosphate buffered saline at 4 . Addition of cryoprotectants and surfactants prevents aggregation of virus particles and extends the shelf life to one year. Lyophilized formulations of both adenovirus and AAV with shelf lives of several years at room temperature have also been described. Although nonviral vectors have been found to be generally robust in standard buffers at 4
. Addition of cryoprotectants and surfactants prevents aggregation of virus particles and extends the shelf life to one year. Lyophilized formulations of both adenovirus and AAV with shelf lives of several years at room temperature have also been described. Although nonviral vectors have been found to be generally robust in standard buffers at 4 , their stability may be extensively influenced by extraneous components included to promote gene targeting. Consider the nature of those components when developing stability protocols and strategies (see below).
, their stability may be extensively influenced by extraneous components included to promote gene targeting. Consider the nature of those components when developing stability protocols and strategies (see below).
ON-SITE PREPARATION AND ADMINISTRATION
One or more product modifications or preparative steps may be required before administration of the gene therapy product to the patient. These modifications or steps are frequently performed close to the time of administration, and, therefore, they are performed under conditions not under control of the original manufacturing facility. The nature of these modifications is dictated largely by characteristics of the product in relationship to the particular application. These include thawing, washing, or filtration to remove unwanted product manufacture-related materials and also include defined physical space with appropriate environmental controls, trained personnel, detailed standard operating procedures, and a comprehensive quality program.
The unique and irreplaceable nature of many gene therapy products, e.g., gene-modified cells, many of which have originated from an autologous or a selected allogeneic tissue source, creates special considerations for product manufacture, release, and administration. Issues pertinent to the administration of cell-based products are addressed in detail in chapter  1046
1046 .
.
On-Site Preparation
Product Manipulations
Before administration, on-site preparation of the gene therapy product may involve one or more manipulations, including the following:
- Change in final container—The manufactured product may have been stored or transported in one container but may require transfer to a different container for administration.
- Change in physical state or temperature—A product may require thawing from the frozen state or warming from the refrigerated state.
- Change in solution or suspension—A product may have to be dissolved, diluted, or suspended in a liquid.
- Addition to biocompatible structural material—A gene therapy product may need to be combined with living, natural, or synthetic structural tissue or matrix. Examples of matrix material include hollow fibers, fibrous sheets, gels, plugs, capsules, sponges, or granules.
- Admixture or compounding with other nonstructural materials—A product may require mixing or compounding with drugs, cytokines, biologics, or other nonstructural materials.
- Filtration or washing—Unwanted materials in the manufactured product, such as particulates, cellular debris, metabolites, or compounds remaining from previous manipulations may require washing or filtration steps.
- Sampling—Sampling of the final product immediately before administration may be required for certain clinical protocols.
Facility Requirements
Facility requirements for performing on-site preparative steps or administration of gene therapy products depend on the nature of the products, their applications, and the manipulations required. The most important determinant of facility features is the level of risk for microbial contamination associated with each step. Definition of low-risk and high-risk conditions can be made according to a framework similar to that defined for Low-Risk-Level Compounded Sterile Preparations (CSPs) and High-Risk-Level CSPs in Pharmaceutical Compounding—Sterile Preparations  797
797 , CSP Microbial Contamination Risk Levels.
, CSP Microbial Contamination Risk Levels.
Release of Final Product
Gene therapy products that undergo on-site preparative steps or manipulations must be subjected to appropriate checks or tests to ensure that all quality specifications are met before release for patient administration. The nature and extent of manipulations will determine whether release requirements or critical specifications must be added to those required immediately after initial manufacture. Pre-release requirements usually include the following:
- Physical inspection of the product, which typically includes measures to ensure appropriate product appearance with regard to color, turbidity, particulates or foreign matter, container integrity; product temperature; and accuracy and convenience of labeling
- Review of process records
- For patient-specific products, clerical checking of product labeling or records related to the identity of the intended recipient.
In addition, products considered to be high-risk products according to the description in chapter  797
797 should undergo additional product testing. For all high-risk products, quality assays for the identity, potency, and purity of the active ingredients should be defined and performed. For high-risk products in Category II, sterility and endotoxin testing should be performed.
should undergo additional product testing. For all high-risk products, quality assays for the identity, potency, and purity of the active ingredients should be defined and performed. For high-risk products in Category II, sterility and endotoxin testing should be performed.
Administration to Patients
Pre-Administration Requirements
Depending on the specific gene therapy application, trained patient-care staff must take steps to prepare the patient for product administration. These steps are aimed at ensuring that the product will provide the intended therapeutic outcome and at minimizing the risk of adverse effects. Issues pertinent to administration of cell-based products are addressed in chapter  1046
1046 . Generally, a thorough re-evaluation of the patient's general condition and suitability for therapy must be performed close to the time of product administration. This evaluation usually includes a patient history, physical examination, and laboratory studies such as blood counts and chemistries. In addition, staff may obtain baseline physical or functional measurements, laboratory tests, or imaging studies relevant to the specific application. Examples include pulmonary function tests for a therapy aimed at improving lung function, measurement of blood levels of an enzyme that is the gene product in a gene therapy application, and nuclear imaging of organs before anticancer therapies.
. Generally, a thorough re-evaluation of the patient's general condition and suitability for therapy must be performed close to the time of product administration. This evaluation usually includes a patient history, physical examination, and laboratory studies such as blood counts and chemistries. In addition, staff may obtain baseline physical or functional measurements, laboratory tests, or imaging studies relevant to the specific application. Examples include pulmonary function tests for a therapy aimed at improving lung function, measurement of blood levels of an enzyme that is the gene product in a gene therapy application, and nuclear imaging of organs before anticancer therapies.
A variety of patient interventions related to route of administration may be required before product administration. For therapies that require intravenous administration, patients with poor peripheral venous access may require placement of a central venous catheter. In applications where gene-modified cells or matrices combined with cells are implanted into the patient, the site of implantation may require preparation in the operating room. This may involve surgically opening the site, removing the degenerated or damaged tissue, trimming of the adjacent tissue to accommodate the implant, and excising the tissue from a second site to be used as an anchor or support for the implant. For instance, in the case of products for wound healing, it is critical that the site for grafting be free from infection and that it demonstrates a well-prepared wound bed. Where gene-modified cells are intended to repair cartilage defects, the site of damage needs to be prepared so that the cells can be applied to a water-tight compartment. For applications involving direct administration of the product into an organ system (for example, bronchioalveolar system) or vascular network (for example, coronary arteries), the patient may require endoscopic or surgical access to these sites.
In all cases, the need for adequate anesthesia and premedication must be carefully evaluated in conjunction with these steps before product administration. Pre-administration patient evaluation must also include assessment of concurrent therapies that may interact with the gene therapy product to modify its effects. Some therapies may be considered adjunctive to the gene therapy, such as cytokines that promote proliferation or differentiation of the infused or implanted tissue. Other commonly used drugs such as antibiotics, antineoplastics, anticoagulants, and anti-inflammatory agents must be evaluated for possible effects on the efficacy of the gene therapy product.
Patient Treatment
Some gene therapy products are patient-specific because they are manufactured from a selected tissue source, such as autologous, selected allogeneic, or xenogeneic tissue. Certain patient-specific products have a defined potential for benefit or adverse immunoreactivity. Systems must be in place to prevent administration of such a product to the wrong patient. Recommended systems include procedures similar to those used for administration of human blood products, including special attention to the correct identification of the patient and patient-specific product by at least two people immediately before administration. These issues are addressed in greater detail in  1046
1046 . Gene therapy products can be administered by a variety of routes. These include parenteral injection, inhalation, and gastrointestinal routes. Other possibilities include direct application of gene therapy products into regional vasculature, organs, tissues, or body cavities by means of needles or catheters or following surgical exposure of the tissue. Although parenteral administration can be accomplished in routine outpatient or inpatient facilities, the other means of administration may require specialized facilities such as an aseptic operating theater or endoscopic suite. In all cases, standard operating procedures and a quality program must be in place to ensure that the product is administered in the intended manner.
. Gene therapy products can be administered by a variety of routes. These include parenteral injection, inhalation, and gastrointestinal routes. Other possibilities include direct application of gene therapy products into regional vasculature, organs, tissues, or body cavities by means of needles or catheters or following surgical exposure of the tissue. Although parenteral administration can be accomplished in routine outpatient or inpatient facilities, the other means of administration may require specialized facilities such as an aseptic operating theater or endoscopic suite. In all cases, standard operating procedures and a quality program must be in place to ensure that the product is administered in the intended manner.
Post-Administration Monitoring of Patient
There should be written policies and procedures for monitoring patient outcomes and managing reports of adverse events. Patient outcome assessment should include indicators that are likely to detect errors or problems related to the entire manufacturing process, with special attention to manipulations, storage, or transportation after the initial manufacture of the product. Management of adverse reactions should include procedures for ensuring prompt medical evaluation and treatment of patients with suspected adverse effects and a system for reporting and evaluating adverse effects that may point to a potential defect in the administered product. Reporting procedures include providing details required for federal, state, or USP adverse-event reporting programs.
Follow-up and monitoring procedures should be implemented for patients who have received gene therapy vectors or ex vivo gene therapies. To the extent that it is relevant and that it can be assessed, vector or gene-modified cell biodistribution and persistence in vivo should be monitored. With direct administration of vectors, localization to the germ line may be an issue. Although preclinical studies can address this issue, useful information may be gained by patient monitoring. When a retroviral vector has been administered, patients should be monitored for replication-competent retrovirus (RCR) according to FDA's Guidance for Industry: Supplemental Guidance on Testing for Replication Competent Retrovirus in Retroviral Vector-Based Gene Therapy Products and During Follow-up of Patients in Clinical Trials Using Retroviral Vectors (October 2000). This involves active monitoring during the first year and archiving of patient samples thereafter if RCR is not detected initially.
Database systems to collate and track patient-monitoring results are essential to management of this information. National registries or publication of data should be considered for establishing the collective safety of gene therapy.
ANALYTICAL METHODS
The complexity and scope of gene therapy products are reflected in the wide range of analytical procedures and their methods that are used to assess product quality. Approved gene therapy products must comply with applicable sections of 21 CFR 211 and 610 to ensure their identity, dose, potency, purity, and safety. Specific guidance for the identification, development, and validation of analytical methodologies to support cell and virus bank characterization, final-product release, and stability studies is currently provided in FDA guidelines for gene therapy manufacturing and testing (see Appendix); in Validation of Compendial Procedures  1225
1225 ; and in the ICH guidelines Q2(R1) and Q6B. Most product-specific analytical methods for gene therapy products have not been standardized. Even well-defined tests such as those described under Sterility Tests
; and in the ICH guidelines Q2(R1) and Q6B. Most product-specific analytical methods for gene therapy products have not been standardized. Even well-defined tests such as those described under Sterility Tests  71
71 may not be directly applicable to certain gene therapy products. For some gene therapy products, large quantities of clinical material may not be available during early clinical development. Some required tests (e.g., sterility) may require modification. Consultation with regulatory authorities is advised.
may not be directly applicable to certain gene therapy products. For some gene therapy products, large quantities of clinical material may not be available during early clinical development. Some required tests (e.g., sterility) may require modification. Consultation with regulatory authorities is advised.
Table 5 provides an overview of product-specific testing parameters for the biological component and general methods or approaches used to satisfy the testing requirements for nonviral, viral, and gene-modified cellular gene therapy products. The analysis of gene therapy products relies heavily on biological assays, but it also uses methodologies developed for biotechnology-derived products. The intent of this section is to outline the types of methods and their specific applications with regard to product characterization, stability, and release testing. Process validation may alleviate the need for certain specific lot-release tests. Development of appropriate reference materials and standards for viral, nonviral, and gene-modified cellular gene therapy products should be a part of product development. Reference materials should be fully characterized in order to provide continuity between standards over time. In the case of gene-modified cellular gene therapy products, the reference material may be a surrogate tissue or simulated product. Reference materials are briefly addressed in the FDA Guidance for Industry: Potency Tests for Cellular and Gene Therapy Products.
Gene-modified cellular gene therapy products may require a rapid-release approach if they have a limited shelf life (see Cellular and Tissue-Based Products  1046
1046 ). The rapid-release approach is not usually applied to viral and nonviral gene therapy products because these products are sufficiently stable for completion of testing before release. Some formulated nonviral gene therapy products also have limited shelf lives. In such cases, the individual components are tested before release and the formulated complex is not tested. The formation and stability of the formulated nonviral gene therapy complex is established via validation studies during product development.
). The rapid-release approach is not usually applied to viral and nonviral gene therapy products because these products are sufficiently stable for completion of testing before release. Some formulated nonviral gene therapy products also have limited shelf lives. In such cases, the individual components are tested before release and the formulated complex is not tested. The formation and stability of the formulated nonviral gene therapy complex is established via validation studies during product development.
As specified in CFR, product samples must be retained after product-release testing is completed. Retain additional samples if rapid-release strategies are employed so that product quality can be reassessed by alternative or traditional test methodologies if necessary.
Table 5. Analytical Tests for Cell and Gene Therapy Biological Products
| Test | Gene-Modified Cellular Gene Therapy Product |
Gene Therapy Products | |
|---|---|---|---|
| Viral | Nonviral | ||
| Identity of Biological Substance |
• Surface marker determination • Species • Morphology • Bioassay • Biochemical Marker |
—Restriction enzyme map —PCR —Immunoassay for expressed gene —Sequencing |
—Restriction enzyme map —PCR —Immunoassay for expressed gene —Sequencing |
| Dose | • Viable cell number • Enumeration of specific cell population • Total DNA • Total protein |
—Particle number —Transducing units (DNA hybridization assay) —Total protein —HPLC assay using authenticated reference standard |
—Plasmid–DNA weight —Formulated-complex weight HPLC or capillary electrophoresis assay using authenticated reference standard |
| Potency | • Viable cell number (cells intended for structural repair) • Bioassays — Colony-formation assay — Function of expressed gene — Induction of secondary effect (e.g., human leukocyte antigen (HLA) induction, secretion of cytokines, and up-regulation of surface marker) |
—Function of expressed gene (induction of secondary effect and other bioassays) | —Function of expressed gene (induction of secondary effect and other bioassays) other bioassays) |
| Purity | • Percentage of viable cells • Percentage of transduced cells • Percentage of cells with specific surface marker • Process contaminants (e.g., serum) |
—Residual host-cell DNA —Process contaminants (e.g., serum and cesium chloride) —Residual helper virus —Optical density ratio —Residual host-cell proteins —Viral protein profile (HPLC assay for defective or immature particles) —Residual RNA |
—Percentage of specific physical form (e.g., percentage supercoiled) —Residual host-cell DNA —Residual RNA —Residual host-cell proteins —Residual solvents —Optical density ratio —Process contaminants (e.g., cesium chloride) |
| Safety | • Mycoplasma • Sterility • Pyrogen and endotoxins • Adventitious viruses • Residual virus • Replication-competent vector |
—General safety —Sterility —Pyrogen and endotoxins —Adventitious viruses —RCV |
—Mycoplasma —Sterility —Pyrogen and endotoxins |
Sampling Issues
Sampling for lot-release testing should be based on the potential distribution for the parameter tested. See Stability Protocol Development under Stability (below) for additional considerations. Samples from each lot should be retained in case of a safety or quality issue with the lot. Even if the product has a very short shelf life, these retained samples can be used to detect impurities and other substances. The need for proper design of the sampling scheme is highlighted in safety testing for adventitious agents or in assessment of RCV for gene-modified cell or viral gene therapy products. In such cases, process validation assists in determining the appropriate statistically based sampling design.
Safety
Safety testing for gene therapy products focuses on three issues: (1) detecting contamination from adventitious sources during product processing, (2) preventing the use of packaging cell lines and plasmids that potentially permit genetic recombination between vectors and the packaging cell lines or plasmids—or among the vectors themselves, and (3) testing the final product to ensure a safe level of undesired genetic and/or structural variants or other viruses used in processing.
The primary means of assessing safety are the performance of biological assays to measure adventitious agents directly. Molecular biology-based assays that measure adventitious agent DNA or RNA or detect undesired genetic variants are also used. Although live genetically engineered vectors officially fall outside its scope, the detailed information available in the ICH Q5A guideline, presented in chapter  1050
1050 , should be consulted because the principles apply.
, should be consulted because the principles apply.
Viral Gene Therapy Products
One of the primary safety concerns associated with viral vectors used for gene therapy is the occurrence of undesired genetic variants. Among them the most critical type, and probably the best studied, is RCV. RCV is more clearly defined for replication-incompetent viral vectors, but for conditionally replication-competent viruses it refers to undesired genetic variants that have lost selectivity toward the target cells and thus might raise safety concerns. Regardless of the virus, these concerns are based on the potential lack of predictability for the pathogenicity of a contaminating virus for a specific route of administration, particularly if it is not the normal route of infection or if humans are not a natural host for the virus. The pathogenesis of a wild-type adenovirus infection is known but may not be predictive for the routes of administration employed with recombinant adenoviral vectors. For replication-incompetent adenoviral vectors, a limit of one RCA per 3 × 1010 viral particles is currently considered acceptable (see the FDA Guidance for FDA Reviewers and Sponsors: Content and Review of Chemistry, Manufacturing, and Control (CMC) Information for Human Gene Therapy Investigational New Drug Applications (INDs)].
Typically, RCA levels are determined by a cell-based assay that allows amplification of the RCA while preventing replication of the product. The cell line most often used for amplification and detection of RCA is the A549 cell line. However, some recombinant adenoviral vectors express therapeutic genes that interfere with analysis on A549 cells. In such cases, a bioassay-based two cell lines is used. The first cell line is chosen on the basis of resistance to the effects of expression of the transgene and with subsequent passage of cell lysate or supernatant onto A549 cells for amplification and detection of the RCA. RCA is most often detected by visual observation of the cytopathic effect, but it can also be detected in the A549 cell culture by immuno- or PCR-based methods.
Quantitation of the RCA level is based on the quantity of sample tested and the detection limit of the assay. Typically, RCA bioassays are validated as being able to detect 1 plaque-forming unit or infectious unit of RCA in the test sample over a wide range of test-sample sizes. Test-sample sizes can range, but they are typically based on the FDA RCA acceptance limit. To verify detection limits, include spike controls as part of the test, even with validated assays. For recombinant adenoviruses produced using HEK293 cells, RCA detection by PCR on the final products or the progeny virus amplified in HEK293 cells can be confounded by detection of residual HEK293 host-cell DNA (detection of the E1 region). PCR assays, however, can be designed to specifically quantitate host cell DNA contamination and can be made specific to particular forms of slow-growing RCA. Quantitative PCR assays can be used in conjunction with a cell-based method for precise quantitation of RCA levels. When a tested sample is found to be positive, the identity of the RCA is usually confirmed by conducting PCR analysis. This rules out the possibility that contamination of the assay by exogenous wild-type adenovirus or other adventitious agents is responsible for the positive result.
For conditionally replication-competent adenoviruses or other replication-competent viral vectors, testing for RCV or undesired genetic variants is usually more complicated and vector specific. Usually one or two nonpermissive cell lines that are not target cells are infected with the replication-competent virus in attempts to produce progeny virus. In order to generate a sufficient quantity of progeny population for analysis, analysts subject the infection to multiple passages and extended culture time. Two normal fibroblast cell lines that are easy to culture, WI-38 and MRC-5, have been used as the model nonpermissive cell lines for detecting RCA in replication-competent adenovirus products. Even after multiple passages on the nonpermissive cell lines, it may be necessary to amplify the progeny (which tend to appear only in minute quantities) in permissive or packaging cell lines to a sufficient quantity for subsequent testing. The resulting progeny should be tested for changes in biological selectivity and genetic composition. Usually the genetic characterization of the progeny population includes restriction enzyme mapping followed by Southern blotting, PCR, or nucleotide sequencing. After the genetic elements unique to RCV or undesired genetic variants are identified, quantitative PCR assays can be designed to monitor the level of RCV after amplification in nonpermissive cell lines or sometimes, if the sensitivity is adequate, directly in the final product without biological amplification. Using a spike control in the biological assay for detecting RCV is encouraged but may not be applicable to all cases. Currently there is no specified acceptable limit of RCA for conditionally replication-competent adenovirus, although clinical safety has been reported for an oncology application with several thousands of RCA per dose.
For retroviral vectors, testing for RCR is required for cell banks, viral vector production lots, and any resulting ex vivo product lots (see FDA's Guidance for Industry: Supplemental Guidance on Testing for Replication-Competent Retrovirus in Retroviral Vector-Based Gene Therapy Products and During Follow-up of Patients in Clinical Trials Using Retroviral Vectors). Standard assays have been designed to detect replication-competent MLV. The pathogenesis and potential long-term toxicity of low-level amphotropic MLV in human beings is not known. Methods commonly used to detect RCR include an amplification of virus titer by application of product to a replication-permissive cell line such as Mus dunni. Because infection is limited by the ability of a virus to reach the cells by means of Brownian motion, procedures (e.g., centrifugation and filtration) that physically bring the virus into contact with the cells can be used to enhance detection. However, high-titer recombinant vector can interfere with the detection of low-level RCR, and this interference may be enhanced by such methods. Infected cells are passaged several times to allow viral replication. Culture medium is harvested at the end of the culture period, and RCR is detected by using an indicator cell line. If the product is an amphotropic MLV, RCR can be detected by using a feline cell-based PG4 S+L– assay, a mink cell-based MiCl S+L– assay, or a marker rescue assay. In S+L– assays, the RCR expresses proteins that lead to transformation and subsequent plaque formation on the monolayer. In a marker rescue assay, RCR infects a cell line that expresses a retroviral vector encoding a marker gene such as 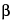 -galactosidase, drug resistance, or a fluorescent protein. The vector is packaged by the proteins supplied to it in trans by the RCR. The potentially vector-laden supernatant is transferred to naive target cells that are then screened for expression of the marker vector.
-galactosidase, drug resistance, or a fluorescent protein. The vector is packaged by the proteins supplied to it in trans by the RCR. The potentially vector-laden supernatant is transferred to naive target cells that are then screened for expression of the marker vector.
Testing for RCR is performed by co-cultivation of the cell line or amplification of vector supernatant with an RCR replication-permissive cell line, typically M. dunni, for several passages. Culture medium is harvested at the end of this co-cultivation process and applied to an appropriate indicator cell line as described above. Note that artifacts may be generated during the co-cultivation assay by expression of an endogenous virus in the permissive cell line or by fusion if the vector-producing cell line is cultured directly with a marker rescue cell line. In addition, co-cultivation may not be possible for ex vivo cell products that have specific culture requirements or limited culture life spans.
Methodologies for testing the presence of RCR in crude, purified bulk or final vector products are not specified. FDA has deposited a reference standard of an amphotropic hybrid MLV with the American Type Culture Collection (ATCC). This viral stock has been assigned a label titer and should be used in assay validation. Method validation should demonstrate the ability to reproducibly detect a single RCR particle in individual product types because the product and its related impurities can interfere with the detection of RCR. Currently, there are no acceptable limits for RCR contamination in products. Any product lot found to contain RCR cannot be used for human use. Reference standards for assessing RCV in other viral vectors including ecotropic, xenotropic, or pseudotyped MLV, adenovirus, and lentivirus have not been developed. The adenovirus reference material, which consists of wild type human adenovirus type 5, has been used as a spike control and during validation of RCA assays, but this practice may not be applicable to all RCA assays. Amplification and detection of replication-competent HIV, especially its pseudotyped variants, may warrant special containment and handling procedures.
Additional safety testing usually focuses on methods similar to those described in Biological Reactivity Tests, In Vivo  88
88 , Safety Tests—Biologicals, and chapter
, Safety Tests—Biologicals, and chapter  71
71 . For viral gene therapy vectors produced using a human cell line, performance of the in vitro adventitious agent bioassays using three cell lines is recommended. For adenoviral vectors, specific tests for adeno-associated virus are also recommended. For adeno-associated virus, specific tests for adenovirus and herpes virus are recommended. Material for testing should be derived from the stage of manufacture that provides the greatest chance of detection, which could be pre-bulk (e.g., late-stage fermentation), the bulk, or the final product.
. For viral gene therapy vectors produced using a human cell line, performance of the in vitro adventitious agent bioassays using three cell lines is recommended. For adenoviral vectors, specific tests for adeno-associated virus are also recommended. For adeno-associated virus, specific tests for adenovirus and herpes virus are recommended. Material for testing should be derived from the stage of manufacture that provides the greatest chance of detection, which could be pre-bulk (e.g., late-stage fermentation), the bulk, or the final product.
Nonviral Gene Therapy Products
Safety testing for undesired genetic variants that might emerge during the manufacturing process in nonviral gene therapy products is similar to that for RCV testing for viral vectors but with more vector-specific considerations. Typically, molecular biology-based methods are applied to the final product to test for variants. When genetic stability is established by process validation, the assays for monitoring the levels of undesired genetic variants may be limited to restriction enzyme mapping followed by further confirmation of critical genetic elements (such as transgenes or regulatory elements) by PCR or Southern blotting.
Dose-Defining Assays
An assay that precisely measures the amount of the product is referred to as a dose-defining assay, and it is selected on the basis of its accuracy and precision. An assay that measures therapeutic activity of the product is referred to as a potency assay, and it is designed to measure product function. The design of the assay depends on the type of product. In the case of chemical and protein drugs, the assays measuring the amount of active ingredient (dose) are referred to as strength assays. Product dose can be defined as the concentration or amount of the drug product administered to the patient, and it is typically measured as product mass.
Particle concentration is a commonly used measure for viral vector product dose. Particle concentration may be measured by physical, biophysical, or in vitro cell-based assays. For example, quantitation of purified adenoviral particles may be determined by using the optical density of a solution of virus in 0.1% (w/v) sodium dodecyl sulfate (SDS) solution at 260 nm, because a relationship between absorption and particle concentration has been published for adenovirus. The particle number concentration is equivalent to the product of the absorbance at 260 nm in a 1-cm cell, the dilution factor, and 1.1 × 1012 particles. A method that has become standard in determining particle concentration is integration of viral peak area of 260 nm and/or 280 nm absorbance against an authenticated reference standard in an anion-exchange resin-based high-performance liquid chromatographic (HPLC) assay. Compared to the optical density method, the HPLC method has the advantage of eliminating the interference of free DNA and/or capsid proteins on quantitation of viral particles. An adenoviral reference material (ARM) from ATCC has an HPLC-determined particle concentration established from a large-scale collaboration that involved many laboratories. Whenever possible, the ARM should be used to calibrate the internal HPLC method and reference material.
Virus concentration can also be assessed by the measurement of selected structural proteins with known molecular masses and known copy numbers within the virion. For this method, the virus must be lysed, and the structural proteins must be separated by using an appropriate, high-recovery chromatographic procedure (e.g., reversed-phase HPLC). The chromatographic separation and the identity and the purity of the selected structural protein must be verified during assay validation by methods such as SDS polyacrylamide gel electrophoresis (SDS-PAGE), peptide sequencing, and mass spectroscopy. The selected structural proteins can be quantified, for example, by integrating chromatographic peaks at 214 nm and comparing the area to that of an authenticated reference standard. The virus concentration can then be calculated based on the molecular mass, the copy number, and the measured mass of the protein. Very importantly, the virus concentration can be estimated simultaneously for multiple structural proteins, which allows the use of this assay in relatively impure virus preparations. This method has been applied to adenovirus and should be applicable to other viral vector types.
Biophysical methods of determining particle number include direct quantitation of vector nucleic acid by radiolabeled-probe hybridization and indirect quantitation by amplification of template nucleic acid (e.g., PCR and RT-PCR) or by signal amplification (e.g., branched-chain DNA using multiple-probe hybridization).
In cases where biophysical methods are not available, bioassays that measure gene-vector titer have been used. These involve infection, transfection, or transduction of a susceptible cell line in vitro, followed by some measure of the product uptake. Methods for quantitation or estimation of the number of infection, transfection, or transduction events include plaque-forming unit assays, tissue culture infectious dose assays based on cytopathic effect of 50% (TCID50) or immunofluorescent detection of an expressed vector protein, or a quantitative DNA-hybridization assay. Examples follow: For replication-competent adenoviral gene therapy products, the ARM available from ATCC has a defined range of TCID50 titer determined via a collaborative effort. Whenever applicable, it should be used in validation of an internal reference standard or assay control of infectious titer assays. However, because of the likelihood of genetic differences between the ARM, which is wild-type human adenovirus type 5, and the replication-competent adenoviral gene therapy product, it may not be reasonable to normalize the titer of the vector of interest to that of the ARM.
For retroviral or lentiviral gene therapy products or AAVs that carry a selectable marker (e.g., that for neomycin resistance) or a reporter gene (e.g., 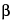 -galactosidase) in addition to the therapeutic gene, the infectious titer is commonly determined by measuring the number of transduced or infected cells expressing these nontherapeutic proteins. Vector titer is typically reported as the number of colony-forming units (cfu) per mL for cells transduced with viral vectors that contain drug-resistance markers and are selected for growth in drug-containing medium. Titer based on
-galactosidase) in addition to the therapeutic gene, the infectious titer is commonly determined by measuring the number of transduced or infected cells expressing these nontherapeutic proteins. Vector titer is typically reported as the number of colony-forming units (cfu) per mL for cells transduced with viral vectors that contain drug-resistance markers and are selected for growth in drug-containing medium. Titer based on 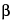 -galactosidase can be expressed in terms of blue cfu per mL after staining and counting the cells that convert the
-galactosidase can be expressed in terms of blue cfu per mL after staining and counting the cells that convert the 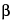 -galactosidase substrate X-Gal into a blue chromophore. For vectors without a marker gene, quantitation of transduction has been measured precisely by using quantitative PCR or has been estimated by hybridization methods.
-galactosidase substrate X-Gal into a blue chromophore. For vectors without a marker gene, quantitation of transduction has been measured precisely by using quantitative PCR or has been estimated by hybridization methods.
Most nonviral gene therapy products contain plasmid DNA, and their usual measure of dose is the DNA mass. The DNA mass may be determined in the formulated state, and, if recombinant protein is included in the formulation, the total combined mass of all formulation components based on a specific ratio can be used. DNA concentrations greater than 500 ng/mL are most simply determined by using optical density measurement at 260 nm. This method is not generally applicable to lipid-formulated DNA. Because RNA and proteins also have significant absorbance at 260 nm, other analyses must be performed to demonstrate minimal contamination with RNA, protein, or residual host-cell chromosomal DNA. Dyes that specifically bind to double-stranded DNA allow accurate measurement of DNA concentrations of less than 500 ng/mL when calculated against an authenticated DNA standard curve. PicoGreen is one such fluorescent dye, and it is minimally affected by single-stranded DNA, RNA, proteins, salts, and detergents. The fluorescent dye Hoechst 33258 also binds to both double-stranded and single-stranded DNA and it can be used to determine DNA concentrations as low as 0.3 ng per mL. The Hoechst 33258 does not bind to protein or RNA, and it can accurately determine the DNA concentrations in crude samples.
Methods such as capillary electrophoresis and HPLC employing an authenticated reference material can also be used to determine the strength of nonviral products.
Potency
Potency is defined as the therapeutic activity of the drug product. Together with dose, potency defines the biological activity of each lot (see Dose-Defining Assays). Potency can be assessed by in vitro or in vivo bioassays. It is not uncommon for these assays to have coefficients of variation between 30% and 50%, although stringent assay design with good statistical consideration could help reduce assay variation. These assays require a well-defined, representative reference material that can be used as a positive control for the assay and/or in calculation of the relative potency of the test article. The general consideration for bioassays in current USP chapters on design and development of biological assays should be applied to the potency assay design for gene therapy products. The positive control qualifies the performance of an individual assay. Potency assay development should focus on characterizing and controlling variability. High-precision assays are more effective tools in monitoring product quality. Information about potency assay variability should be incorporated into the stability study design and the proposed statistical approach to assignment of expiration date (see Stability).
Bioassays employed to measure the potency of viral and nonviral gene therapy products generally involve infection, transfection, or transduction of a susceptible cell line in vitro, followed by some functional measure of the expressed gene of interest. Functional assays for the therapeutic gene (e.g., those measuring enzyme activity and cell growth stimulation or inhibition) should generally be used instead of analytical methods such as enzyme-linked immunosorbant assay (ELISA). When the biological function of the expressed transgene exhibits a broad range of activities or only generates semiquantitative results, the ELISA or other immunological or biochemical readouts can be used as a surrogate potency assay with a tight specification range if extensive characterization data is available to demonstrate that all expressed protein is biologically active. For example, in the case of a gene therapy product expressing a cytokine, cytokine expression is usually quantified by ELISA first, and the result is used to adjust the sample dilution for the functional assay. The potency of such vectors may be better controlled by the ELISA quantitation results, but the biological activity of expressed cytokine could be used to verify that the measured mass is biologically active without the requirement to meet a narrow specification range for the biological activity itself.
HPLC or flow cytometry, which provide information about the level of expression but only infer function, have also been used in a context like that described for immunoassays. In addition, for viral vectors, infectious titer measurements by themselves are generally not considered an adequate measure of product potency. For example, the TCID50 titer or plaque-forming-unit assays for adenoviral vectors on HEK293 cells can indicate that the infectivity of adenovirus is preserved but do not confirm that the adenoviral product has maintained full biological function(s), especially transgene biological activity. The design and ultimate suitability of an assay system for determining product potency depends on the relationship between the intended human target cell in vivo and the following: (1) the transduction or transfection efficiency of the cell line used in vitro; (2) the protein expression levels; and, (3) the duration of expression required for the therapeutic effect.
In vivo tests can also be used to measure vector-product potency. Readouts can be based on a response per animal (e.g., blood levels of therapeutic protein 24 hours after treatment) or a group response rate (e.g., percentage of animals that elicited an immune response or survived virus challenge). The availability of an appropriate in vivo test system depends on the vector-host range (for viral vectors), the pharmacokinetics and biodistribution of the vector and the resulting gene product relative to its human counterpart, and the time frame required to observe the therapeutic effect or surrogate. Issues of cost, facilities, validation, and ethics determine the practicality of an in vivo potency test.
Purity
Analytical methods that separate, isolate, and specifically quantify the intended active product components determine product purity. Impurities are either product- or process-related components that can be carried through to the final product. The manufacturing and purification process should be optimized to consistently remove impurities while retaining product activity. The requirement to test for a particular impurity for product lot release depends on the following: (1) the demonstrated capability of the manufacture and purification process to remove or inactivate the impurity through process validation, and (2) the potential toxicity associated with the impurity.
Examples of process-related impurities associated with gene therapy products include residual production-medium components (e.g., FBS, antibiotics, cytokines, and E. coli chromosomal DNA in a plasmid product), ancillary products used in downstream processing (e.g., nucleases such as DNase I), and residual moisture for lyophilized vector products. Impurities may be bioactive (e.g., cytokines and hormones) or immunogenic (e.g., product aggregates, degradation products, plasmid-selection markers, and nonhuman-derived proteins), or they may have other deleterious effects (e.g., they may compete with the product) if administered at a dose equal to that of the product. Product-related impurities are specific to each product type. Examples include nicked plasmid forms in nonviral products and defective or immature virus particles in retroviral or adenoviral vector products. Analytical methodologies to assess purity require quantitation or physical separation of intended product from its impurities. Common sense should drive the need to quantify specific impurities. Suitable validation of the manufacturing process may limit the need for specific lot-release testing for impurities. Manufacturers may place an emphasis on demonstrating the consistency of the product-impurity profile.
Testing for impurities is often extensive during product characterization and process validation when the consistency of the manufacturing and purification process is being demonstrated. Testing for impurities as part of lot-release testing should reflect the safety risks associated with the impurity and the ability of the process to consistently remove that impurity.
Viral Gene Therapy Products
Product-related impurities for viral vectors include aggregates and defective and immature particles that may be produced during the manufacture or purification of the recombinant vector. Aggregates of vector may form if the product is highly concentrated, stored under certain conditions (e.g., under a certain pH or temperature), or reconstituted after lyophilization. Assays to detect aggregates include particle size analysis by laser light-scattering and the use of nonreducing, nondenaturing PAGE, followed by staining of the gel or transfer and detection of viral proteins by Western blot analysis. Sedimentation rate analysis also allows separation of aggregates from monomers based on size. Optical density analyses of light scattering are also used to assess vector aggregation.
Defective particles are viral particles that do not contain the appropriate recombinant genome—that is, they contain some other nucleic acid or contain no genome at all, or the vector has some missing, defective, or otherwise altered structural component that impairs its ability to transduce a cell. For viral vector systems that have capsomeric symmetry that requires the appropriate nucleic acid incorporation for configuration, empty particles may be readily distinguished from those carrying genomes. For enveloped viruses, empty particles may not be as readily separated from those with encapsidated nucleic acid.
For some viral vector products, active viral particles can be separated from defective particles by using analytical HPLC. Anion-exchange resins have been used to separate active adenovirus from defective virus particles. However, this method might not be useful for an adenoviral vector purified by anion-exchange chromatography unless the resin for the assay is different from that used during manufacture. Depending on the nature of the viral vector and its nonactive or defective forms, other methods of separation, such as equilibrium centrifugation in a cesium chloride density gradient, may need to precede the quantitation of the active particle. Ideally, the method of separation will allow quantitation.
Defective particles that carry a non-cell-derived oncogene or other undesirable genes may pose a special concern. For example, in murine-based retroviral packaging cell lines, small viral elements called VL30 sequences can be packaged in about one-third of all particles. Assays may be needed to quantify specific defective particles if they are known to be present in quantities sufficient to pose a safety concern.
Virus quality and the comparability of preparations can also be assessed by measuring selected structural proteins with known molecular masses and known copy numbers within the virion. For this method, the virus is lysed, and the structural proteins are separated by using reverse-phase HPLC or some other high-recovery chromatographic procedure. The chromatographic separation should be validated, and the identity of the selected structural proteins should be verified by methods such as SDS-PAGE, peptide sequencing, or mass spectroscopy. Fingerprinting of the batch can be conducted based on quantification of the selected structural proteins and comparison to a reference standard. When the method incorporates mass spectroscopy, impurities such as structural variants can also be identified. For adenovirus preparations, some precursor and most mature virion proteins can be detected and distinguished, thus allowing monitoring of the product and of the immature virion forms.
Host cell-derived proteins may be considered impurities for some viral vector products and may be separated and quantified by PAGE or HPLC or detected by amino acid analysis, Western blot, or immunoassay-based methods. However, for enveloped viruses such as retroviruses, host cell-derived membrane proteins are an integral part of the product. In those vector systems, it may be difficult to determine the presence of contaminating exogenous host-derived proteins.
Presence of specific process-related impurities depends on the manufacture and purification process of each vector or product type. However, most products need to be tested for residual endotoxins (see Bacterial Endotoxins Test  85
85 ). Acceptable limits of endotoxins have been determined and can be directly applied to viral vector products. Although genomic DNA derived from continuous cell substrates used to manufacture biological product historically has been considered potentially tumorigenic, recent studies suggest that the risks are very low. However, every attempt should be made during process development to reduce levels of contaminating DNA. The need to test for residual DNA as part of product lot release should be evaluated on a case-by-case basis and may depend on the size distribution of the DNA, its association with the product or its formulation components, and the product's route of administration. Quantitative PCR assays can analyze the amount of residual host-cell DNA by using primers designed to amplify evolutionarily conserved and abundant target sequences such as 18S for HEK293 cells.
). Acceptable limits of endotoxins have been determined and can be directly applied to viral vector products. Although genomic DNA derived from continuous cell substrates used to manufacture biological product historically has been considered potentially tumorigenic, recent studies suggest that the risks are very low. However, every attempt should be made during process development to reduce levels of contaminating DNA. The need to test for residual DNA as part of product lot release should be evaluated on a case-by-case basis and may depend on the size distribution of the DNA, its association with the product or its formulation components, and the product's route of administration. Quantitative PCR assays can analyze the amount of residual host-cell DNA by using primers designed to amplify evolutionarily conserved and abundant target sequences such as 18S for HEK293 cells.
Quantitation of residual serum components such as bovine serum albumin (BSA) can be achieved by using ELISA and a BSA reference standard. Researchers may need to develop specific functional or immunological methods for other ancillary products, including other culture media or purification process components such as cytokines or enzymes (e.g., deoxyribonuclease 1 or benzon nuclease).
Nonviral Gene Therapy Products
A plasmid used as a drug substance is considered a well-characterized biologic, and key impurities from the manufacturing process are well known. Testing is usually performed on each individual component: the plasmid DNA, lipid or lipoplex reagents, and protein components if any are present in the formulation. Plasmid DNA is characterized for a variety of impurities, including residual host-cell DNA, residual RNA, and residual protein. Residual protein testing is frequently included in lot-release testing. Optical density ratios (usually the measurement at 260 nm to that at 280 nm) are frequently used in purity specifications for plasmid DNA.
In addition, the plasmid DNA should also be characterized with regard to its conformation in solution. Plasmid DNA exists as monomeric supercoiled, relaxed monomer, and linear forms. Because all forms can be generated during large-scale fermentation, and data about their relative in vivo potency is scarce, the relative quantity of each form is monitored to verify batch-to-batch consistency in the relative amounts of each conformation. Agarose gel electrophoresis can resolve each of these forms but is not highly quantitative for each individual species. Analytical anion-exchange HPLC serves as a quantitative assay for monomeric supercoil and other forms, including concatamers. Other analytical methods that have been valuable for characterization of plasmid constructs during process development and validation such as capillary gel electrophoresis, linear-flow dichroism, and atomic-force microscopy are also viable methods to assess the purity of a given plasmid preparation. The most appropriate method for lot release depends on how each plasmid conformation affects product potency. Specific details for each of these methods are outlined in Nucleic Acid-Based Techniques—General  1125
1125 .
.
Tests should be conducted for process-related impurities such as residual organic solvents (phenol, alcohol), salts, and certain antibiotics such as kanamycin used during the fermentation process. Lipid and lipoplex formulation components must also be tested for their chemical purity. Testing for specific chemical impurities is commonly performed by using gas chromatography–mass spectroscopy (GC–MS), HPLC, or thin-layer chromatography (TLC) methods. If protein is part of the formulated complex, then the protein must also be tested for purity. HPLC is capable of detecting trace amounts of residual antibiotics and can therefore be used during process validation or lot-release testing to confirm that they have been effectively removed. The specifics of these methods are outlined in Biotechnology-Derived Articles—Peptide Mapping  1055
1055 or in Biotechnology-Derived Articles—Total Protein Assay
or in Biotechnology-Derived Articles—Total Protein Assay  1057
1057 .
.
Bacterial protein, DNA, RNA, and endotoxins are the major types of host-derived process contaminants. Standard protein assays (e.g., Lowry, Bradford, or Coomassie), PAGE followed by silver staining or Western blot analysis, or ELISA can be used to detect residual host protein in the nanogram range. Host chromosomal DNA can be detected by slot blot hybridization (detection in picogram range) or by real-time PCR (detection sensitivity < 1pg) using highly conserved target sequences (e.g., 18S for E. coli). PCR assays for this purpose must use recombinant polymerases that are highly purified to minimize residual bacterial DNA for which the presence can create background signals. PAGE or agarose gel electrophoresis followed by fluorescent dye staining can be used to detect residual RNA. Quantitation may not be required because of the labile nature of RNA and the low-level toxicity associated with it. The Limulus amoebocyte lysate (LAL) test is the most sensitive and widely used method for endotoxins determination. Colorimetric assays offer sensitivities of 0.005 EU/mL. Details of the methods described here are outlined in  1057
1057 , Biotechnology-Derived Articles—Polyacrylamide Gel Electrophoresis
, Biotechnology-Derived Articles—Polyacrylamide Gel Electrophoresis  1056
1056 , Nucleic Acid-Based Techniques—Approaches for Detecting Trace Nucleic Acids
, Nucleic Acid-Based Techniques—Approaches for Detecting Trace Nucleic Acids  1130
1130 ,
,  1125
1125 , and
, and  85
85 .
.
Lyophilized Viral and Nonviral Vector Products
Residual moisture can affect the stability of a lyophilized vector product. FDA's Guideline for the Determination of Residual Moisture in Dry Biological Products recommends a 1% residual moisture level, although data indicating no adverse effects on product stability at higher levels is considered acceptable. Residual moisture levels can be determined by using a standard method (see Water Determination  921
921 ) that is compatible with the formulated product.
) that is compatible with the formulated product.
Identity
Lot-release testing for gene therapy products must include an identity test. This test clearly identifies the product and confirms that inadvertent substitution with another product has not occurred. The complexity of the identity test depends on the nature of the specific product and the array of products being manufactured. For example, more extensive and rigorous testing may be performed for an autologous gene-modified cell therapy product at a facility where multiple patient products are manufactured than for a viral vector product produced at a site that manufactures a single vector product.
Viral Gene Therapy Products
For characterization purposes, restriction enzyme mapping and sequencing of the transcription unit DNA are the most commonly used approaches. PCR-based methods, restriction enzyme mapping, and transgene-expression-based immunoassays are commonly used to confirm the identity during lot-release testing.
Nonviral Gene Therapy Products
Restriction enzyme mapping is the most common identity method for plasmid-based products. The number of enzymes used to create the vector fingerprint will vary according to the complexity of the DNA and the degree of similarity between multiple products. If lipids, lipoplex agents, or proteins are used to formulate the DNA, then their identity must also be tested and confirmed. Lipids and lipoplex components may be identified by procedures used for traditional pharmaceuticals, such as GC–MS and TLC. Protein components of the formulation may be identified by peptide mapping or other means outlined under  1057
1057 .
.
STABILITY
The shelf lives of gene therapy products vary widely depending on the nature of the product, its intended clinical use, its specific attributes, and the recommended storage, packaging, and shipping conditions. Therefore, it is difficult to draft uniform guidelines regarding stability-study duration and testing frequency for all products. In all cases, the study should be designed on the basis of scientifically sound principles and approaches and a comprehensive understanding of the final therapeutic product and its intended use. The product's stability during in-process hold steps, cell and virus banks, critical raw materials, and reference standards also must be assessed. A well-designed and executed stability program will provide a high degree of assurance that the product is stable within the specified shelf life.
For viral and nonviral vector gene therapy products and gene-modified cellular gene therapy products that are not patient specific, the selection of batches to support license application and final-product labeling should be carried out in accordance with the principles of stability testing, such as those described in ICH guideline Q5C and chapter  1049
1049 . Stability data should also be collected for bulk material and at other in-process points if material is stored before final processing and filling. Issues related to the stability of cell-based products are addressed in chapter
. Stability data should also be collected for bulk material and at other in-process points if material is stored before final processing and filling. Issues related to the stability of cell-based products are addressed in chapter  1046
1046 .
.
Nonviral DNA plasmid vectors are often formulated with specific mixtures of lipids, proteins, or lipoconjugates to form liposomes or encapsulated complexes. Depending on the formulation, a shelf life of hours to years can be attained. Where a product has a short shelf life, the final formulation may require preparation at the clinic just before administration. Instability is frequently observed as aggregation and precipitation. Formation and stability of the formulated complex should be characterized and established by validation studies during product development. Stability data should also be collected for major components of the formulated complex, such as the lipids, the liposomes, and the DNA itself.
Stability-Protocol Development
Stability studies verify that the storage conditions maintain the purity and potency of the product for a defined period so that product administered to the patient is still capable of meeting the stability specifications. These specifications may differ from the manufacturing release specifications, but they must be verified with clinical data. Formal stability studies to support licensure as well as plans for gathering early-phase product stability information should be detailed in a written plan that describes how data will be collected and analyzed to support the product's expiration period. Protocols should follow the format recommended in existing guidelines and should include the scope, storage conditions, number of lots that will be tested, test schedule, assays that will be used, data analysis, and product specifications. Any assay used in a formal stability study for licensure must be validated before the study begins. The specific study design should take into account the problems the product may encounter during manufacturing, shipping, and processing at the clinical site (see Accelerated and Most Appropriate Challenge Conditions, below). The study design should also incorporate the latest knowledge in the biological sciences and should address existing regulatory requirements. For instance, if the product's final formulation is performed at the clinical site, stability studies on this final formulation should be performed to establish the time and conditions under which the product can be held.
Stability assessment should include an evaluation of product functionality (potency). The potency assay often has a high degree of inherent variability. Measuring and calculating the decay of product activity by employing the standard statistical methodologies may require multiple, frequent sampling intervals over an extended period of time and may require analysis of more than three production lots to compensate for assay variability. Initial studies to establish a provisional expiration date must be conducted before administration to the first patient. Initial studies are also useful for determining which assays are stability indicating, that is, the best indicators of product degradation. Because existing compendial methods do not address the unique characteristics of gene therapy products, the development of assays that would address these unique characteristics is encouraged.
Accelerated and Most Appropriate Challenge Conditions
The stability-indicating profile of a gene therapy product varies over time under the influence of a wide variety of environmental conditions, including temperature, extremes in physiological storage conditions, and light. Multifactorial degradation pathways must be considered when researchers investigate the effects of these parameters on the stability of the product. Studies should include conditions that are outside the specified storage ranges, that is, challenge conditions such as those encountered during periods of abnormal storage, shipping, or handling. Examples include brief incubator malfunctions, incubator or cold storage failure, periods of extreme temperature fluctuation due to shipping to hot or cold climates, hypobaric conditions experienced in the cargo hold of a commercial airliner, or temperatures likely to be encountered in the surgical suite. A short exposure to an environmental condition well outside of an established limit and a long exposure to an environmental condition just outside of an established acceptable range may be equally detrimental to the overall stability profile. The slow and constant rate of product degradation at a specified temperature may increase if a different set of storage conditions is applied. The effect of light on the stability-indicating profile should be investigated if it is scientifically warranted. Give special attention to products stored in fluids that contain light-sensitive or reactive components that may give rise to cytotoxic by-products.
Studies analogous to accelerated aging studies typically used in pharmaceutical stability-monitoring programs are also useful to determine how the product degrades and which assays are stability indicating. These studies can be the same as some of those mentioned in the preceding paragraph. Other studies include placing a product at 37 , or at 18
, or at 18 when its normal storage temperature is 25 ± 2
when its normal storage temperature is 25 ± 2 , or placing a lyophilized product in a high-humidity environment. Such studies should be performed before formal stability studies begin so that the latter can incorporate the validated stability-indicating assays.
, or placing a lyophilized product in a high-humidity environment. Such studies should be performed before formal stability studies begin so that the latter can incorporate the validated stability-indicating assays.
STORAGE AND SHIPPING
Appropriate conditions are chosen to preserve the purity and potency of the product so that its specification and those of its ingredients are maintained throughout storage, shipping, and handling at the clinic. Initial studies must be conducted before patient administration to determine acceptable storage, shipping, and handling conditions. The initial storage and shipping conditions need not be those envisioned for the commercial product but should ensure that the product specifications are maintained beyond the initial expiration date. For products with short shelf lives, storage and shipping conditions, even within a medical center, must be considered at the same time because shipping constitutes the bulk of storage time after manufacturing. Give special consideration to the ability of gas to permeate the shipping container, especially if the gene therapy product is stored or shipped on dry ice. Once stability-indicating methods are developed and the final storage and shipping conditions are chosen, these must be validated as discussed under Stability.
Most products with limited shelf lives are shipped by reliable overnight courier systems. In some cases, highly fragile products are hand-carried onto commercial aircraft. Special permission must be obtained by commercial carriers if scanning by airport X-ray equipment must be avoided. Cargo shipping studies should be designed during the development of packaging systems to identify stresses to which the product may be subjected. Bracing and insulating materials should then be chosen and validated to provide a packaging system that will tolerate, and protect the product against, the extreme conditions of shipping.
Most gene therapy products can be either lyophilized or formulated by means similar to those employed for many recombinant proteins or cell therapy products. These storage formulations typically have expiration periods longer than one year and no unusual shipping requirements. Nonviral gene therapy products, which may be unstable in their final formulation, can have similar expiration periods if they are stored in a multiple-vial kit with the nucleic acid in one vial and a carrier, such as lipids, in the other. The final formulation is performed at the medical center just before administration.
LABELING
Product labeling is regulated by the FDA, and compliance with existing policies is required. Because gene therapy products are regulated biologics, their labeling is subject to these rules. Biologics and devices must meet labeling requirements specific to the container and the package (21 CFR 610 and 801, respectively). Both the container label and the package label must include the expiration date. If the container is packaged, then the recommended storage conditions should be included on the outer package label. If the container is not packaged, the recommended storage conditions and all other requirements of a package label must appear on the container. Labeling must also comply with relevant national and international requirements.
If a product must be applied to the patient in a particular physical orientation or in a specifically defined area, labeling that indicates the correct orientation and/or area should be apparent even after the package is opened. Unless the product has been screened for pathogenic or microbial contaminants before release, appropriate biohazard labeling may be required. For products with very short shelf lives, expiration dating requires adjustment and correction for time zones to provide the user an accurate assessment of shelf life. Clinical procedures must be scheduled around these crucial time frames. For patient-specific products, the patient's full name, initials, or a combination of these will need to appear on the labeling, in addition to lot designation, to ensure that the product is administered to the appropriate patient.
REGULATIONS AND STANDARDS
The technologies involved in manufacturing gene therapy products have been widely documented in the literature and continue to evolve. These products can be regulated as drugs or biologics, or uncommonly as devices, depending on how they are manufactured and used. The novel approaches permitted by these technologies may make it difficult to determine which FDA centers will be involved in their regulation, and the FDA has advised manufacturers to seek clarification in the early stages of development. Currently, the Center for Biologics Evaluation and Research (CBER) regulates most human gene therapy products. CBER relies on both the Public Health Service Act and the Federal Food Drug and Cosmetic Act. Regulation is the same as that for biotechnology-derived products. The general requirements are described primarily in 21 CFR. The federal government has issued many guidance documents as Points to Consider or Guidelines (see www.fda.gov and, in particular, www.fda.gov/cber/publications.htm). ICH guidance documents for many of the quality-related areas are relevant in varying degrees to qualifying gene therapy products (although some products are nominally outside the scope of the guidance documents, the principles still apply; see www.ifpma.org or www.ich.org). Some of these documents are reproduced in USP–NF as general chapters. ICH has also held a number of meetings about gene therapy products and has a Gene Therapy Discussion Group (GTDG) that addresses current issues in gene therapy product development and research and has released several ICH Considerations that reflect harmonized principles. The National Institutes of Health (NIH) has published Guidelines for Research Involving Recombinant DNA Molecules that require NIH review of research, including clinical research or trials conducted or sponsored by institutions that receive NIH funding. These guidelines apply to many gene therapy products.
Biological and biochemical standards for QA of the production and analysis of gene therapy products are highly desirable. The diversity of gene therapy products, in particular viral vectors, has so far limited the development of standards that have wide applicability. A MuLV RCR preparation (VR-1450) with an assigned infectivity titer is available from ATCC for testing murine retroviral vectors for the presence of RCR. A wild-type adenovirus type 5 reference standard with assigned particle number and infectivity titer for characterization of adenoviral vectors is also available from ATCC. A working group has been set up to oversee the development of an AAV reference standard. However, several obstacles to choosing, developing, establishing, and circulating suitable standards are apparent. These include decisions about which virus serotype will be most commonly and successfully used for gene therapy, availability of GMP prepared materials, safety, long-term stability, transportation, and initiation and completion of collaborative studies to evaluate candidate standards. Thus, development of standards for other viral vectors, including lentiviral-, herpes viral-, and poxviral-vectors, remains challenging.
New methodologies, including proteomics, novel nucleic acid technologies (NATs), protein modification methods, and stem cell isolation and culture, are now available and, in many cases, are applicable to the development, characterization, and analysis of gene therapy products. In addition, the use of synthetic polymers both for the modification of existing viral vectors and for the development of chemically dynamic synthetic vectors provides advantages, e.g., improved systemic circulation, better targeting and delivery, and lower levels of immunostimulation and inflammation. The availability of defined stem cell populations and improved engrafting methods should lead to greater effectiveness of ex vivo transduced cells used in gene therapy protocols. The introduction of new methodologies will require the continual review and regulatory oversight to ensure the quality and safety of gene therapy products of the future.
APPENDIX
Gene therapy products are regulated by the FDA as biologics, and therefore their manufacturing, testing, labeling, and other factors are subject to the requirements codified in CFR and FDA guidance documents (www.fda.gov). Additional guidance is provided in ICH guidelines (www.ich.org). Manufacturers of gene therapy products that seek markets outside the United States should refer to regulatory documents from relevant countries. Beyond USP chapters, the following list includes regulatory documents, as well as best practices for the development, manufacturing, quality control, and quality assurance of gene therapy products:
CFR
21 CFR 210
21 CFR 211
21 CFR 600s
21 CFR 610 Subpart G
21 CFR 801
21 CFR 820
FDA Guidance Documents
Guideline for the Determination of Residual Moisture in Dried Biological Products (January 1990)
Guidance for Industry: Human Somatic Cell Therapy and Gene Therapy (March 1998)
Guidance for Industry: Supplemental Guidance on Testing for Replication-Competent Retrovirus in Retroviral Vector-Based Gene Therapy Products and During Follow-up of Patients in Clinical Trials Using Retroviral Vectors (October 2000)
FDA Guidance for Industry: Investigating Out-of-Specification (OOS) Test Results for Pharmaceutical Production (October 2006)
Guidance for FDA Reviewers and Sponsors: Content and Review of Chemistry, Manufacturing, and Control (CMC) Information for Human Gene Therapy Investigational New Drug Applications (INDs) (April 2008)
Draft Guidance for Industry: Potency Tests for Cellular and Gene Therapy Products (October 2008)
National and International Regulatory Documents
Q5A(R1): Viral Safety Evaluation of Biotechnology Products Derived from Cell Lines of Human or Animal Origin
ICH Q5C: Quality of Biotechnological Products: Stability Testing of Biotechnological/Biological Products
ICH Q5D: Quality of Biotechnological Products: Derivation and Characterization of Cell Substrates Used for Production of Biotechnological/Biological Products
ICH Q6B Specification: Test Procedures and Acceptance Criteria for Biotechnological/Biological Products
ICH Q2 (R1): Validation of Analytical Procedures: Text and Methodology
NIH Guidelines for Research Involving Recombinant DNA Molecules (http://www4.od.nih.gov/oba/guidelines.html)
GLOSSARY OF TERMS
Adenovirus—
Virus belonging to the family Adenoviridae of DNA viruses having a nonenveloped virion with 252 capsomeres and a diameter between 70 and 90 nm; a single linear molecule of double-stranded DNA (36 to 38 kb); at least 10 structural ether-resistant and acid-stable proteins; virions are released by cell destruction.
Adenovirus-Associated Virus (AAV)—
Human parvovirus contains a single-stranded DNA genome and depends on helper viruses (adenovirus, herpes virus, or vaccinia-virus) for replication. Without co-infection, the wild-type virions integrate at a specific site on chromosome 19 and remain latent.
Adventitious Agent—
A foreign agent that is introduced accidentally or inadvertently; not natural or hereditary (as in microbial, chemical, or biochemical contamination of a purified substance).
Amphotropic Virus—
A virus that infects and replicates in cells from multiple species.
Ancillary Materials—
Components used during manufacturing that are not intended to be present in the final product. Examples: growth factors, monoclonal antibodies, cell-separation devices, and media components.
Autologous—
From one's own body.
Base Pair—
Two nucleotide bases on different strands of the nucleic acid molecule that bond together.
Bioassay—
Measurement of the effectiveness of a compound by its effect on animals or cells in comparison with a standard preparation. (See also Potency.)
Biological Product—
Any virus, therapeutic serum, toxin, antitoxin, or analogous product applicable to the prevention, treatment, or cure of diseases or injuries in humans. (In this US FDA-derived definition, the term analogous product has been interpreted to include essentially all biotechnology-derived products and procedures including gene therapy, transgenics, and somatic cell therapy.)
Biotechnology—
Any technique that uses living organisms (or parts of organisms) to make or modify products, to improve plants or animals, or to develop microorganisms for specific uses. The newer definition refers to the industrial and pharmaceutical use of rDNA, cell fusion, novel bioprocessing techniques, and gene therapy.
Cell Lines—
Cells that are derived from primary culture embryos, tissue, or organs. Such cell lines may have a finite life span or may be immortalized (modified to be able to replicate indefinitely).
Cell Therapy—
Therapy that uses whole cells to treat a disease, condition, or injury. Distinct from tissue and organ transplantation.
CFTR—
Cystic fibrosis transmembrane conductance regulator.
cGMP—
Current good manufacturing practices. FDA outlined cGMPs in the 21 CFR, and in the Federal Register, and its Points to Consider.
Complementary DNA (cDNA)—
DNA synthesized from an mRNA rather than a DNA template. It is used for cloning or as a DNA probe for locating specific genes.
Cytokine—
Any factor that acts on cells; usually a protein that promotes growth.
Cytoplasm—
Cellular material that is within the cell membrane and surrounds the nucleus.
Cytotoxic—
Able to cause cell death.
Differentiation—
A process of biochemical and structural changes by which cells become specialized in form and function.
Ecotropic Virus—
A virus that infects and replicates in cells from only the original host species.
Electroporation—
Method for enabling transfer of material into cells that involves use of a brief electrical field to create temporary pores in the cell membrane.
ELISA—
Enzyme-linked immunosorbent assay. An immunoassay that utilizes an enzyme-labeled antigen or antibody to detect the binding of a molecule to a solid matrix.
Enveloped Viruses—
Viruses containing a lipoprotein bilayer surrounding the capsid and acquired by budding through the cell membrane of the host cells.
Episomal—
Pertaining to any accessory extra-chromosomal genetic material.
Ex Vivo—
Procedure performed outside of the living organism.
Fluorescence-Activated Cell Sorter (FACS)—
A machine that sorts cells based on fluorescent markers attached to them.
Formulated—
Prepared in accordance with a prescribed method or conditions.
Fusion—
Joining of the membrane of two cells, creating a daughter that contains some of the same properties from each parent cell. It is used in making hybridoma cells in which antibody-producing cells are fused to mouse myeloma cells.
Gene Construct—
Expression vector that contains the coding sequence of the protein and the necessary elements for its expression.
Gene Therapy—
Therapy that uses nucleic acid that is subsequently expressed as RNA or protein to treat a disease or condition. The US FDA defines gene therapy products as products containing genetic material administered to modify or manipulate the expression of genetic material to alter the biological properties of living cells.
Genome—
Total hereditary material of a cell.
Germ Cell—
Reproductive cell (sperm or egg), gamete, or sex cell.
Graft-Versus-Host Disease (GVHD)—
Rejection of the transplanted tissue by the host. It is the leading cause of patient death when mismatched allogeneic tissue is used.
Growth Factors—
Factors responsible for regulatory cell proliferation, function, and differentiation.
Helper Virus—
Aids the development of a defective virus by supplying or restoring the activity of a viral gene or by enabling the defective virus to form a functional envelope.
Hematopoietic—
Pertaining to or affecting the formation of blood cells.
Hepatocyte—
The predominant cell type in the liver that has an important role in metabolism and is a source of serum proteins. These cells generally do not divide, but when injured they can divide and regenerate until the injured cells are replaced.
Herpes Simplex Virus (HSV)—
A DNA virus that is a member of the family Herpesviridae. It can infect both warm- and cold-blooded vertebrates by contact between moist mucosal surfaces.
Human Leukocyte Antigen (HLA)—
Proteins controlled by the major histocompatibility complex. These proteins play a key role in determining transplant compatibility.
Humoral—
Pertaining to elements found in body fluids (for example, humoral immunity and neutralizing antibodies).
Hybridization Dot Blot (DNA or RNA)—
A technique for detecting, analyzing, and identifying protein; similar to the Western blot but without electrophoretic separation of proteins.
Immunoassay—
Technique for identifying substances based on the use of antibodies.
Insertional Mutagenesis—
A type of mutation that is caused by the insertion of nucleic acid into a host-cell chromosome. There are multiple possible negative consequences of such an event, including death of a cell if an essential gene is inactivated or predisposition to cancer if a tumor suppressor gene is inactivated.
Integration—
Assimilation (insertion via covalent binding) of genetic material (DNA) into the chromosome of a recipient cell.
Intrabodies—
Intracellular antibodies that are not secreted and that are designed to bind and inactivate target molecules inside cells.
In Vivo—
Procedure performed in the living organism.
In Vitro—
Procedure performed outside of the living organism. It may involve cells or tissues derived from the organisms.
Leukemia—
Malignant neoplasm of the blood-forming tissues.
Lipoplex—
A formulation of lipids and polymers and/or proteins.
Liposome—
A spherical lipid bilayer enclosing an aqueous compartment.
Mock Run—
A test run that deliberately omits some critical reagents.
Monoclonal Antibodies—
Antibodies that are derived from a single cell clone.
Naked DNA—
Isolated, purified, and uncomplexed DNA (no protein or lipid).
Oligonucleotide—
A polymer consisting of a small number of nucleotides, usually 5 to 30.
Oncogenes—
Genes associated with neoplastic proliferation (cancer) following a mutation or perturbation in their expression.
Oncogenic—
Cancer-causing.
Packaging Cell Line—
Cell line that produces proteins required for packaging and production of viral vectors in an active form but does not produce replication-competent virus. It complements at the protein level what the vector is lacking genetically.
Parvovirus—
DNA viruses of the family Parvoviridae. Host range includes many vertebrate species. Small, linear chain, single-stranded DNA with terminal hairpin loops.
Plasmid—
A small circular form of DNA that carries certain genes and is capable of replicating independently in a host cell.
Process Validation—
Means for providing documentation that the manufacturing process is controlled, reproducible, and capable of consistently producing a product that meets predetermined specifications.
Producer Cell Line—
An established cell line used to produce virus vectors, often at a large scale.
Polymerase Chain Reaction (PCR)—
Technique to amplify a target DNA or RNA sequence of nucleotides by repeated cycles of polymerase-based copying, resulting in geometric increases in copy number.
Potency—
A quantitative measure of biological activity based on the attribute of the product linked to the relevant biological properties.
Promoter—
DNA sequence that is located at the front of a gene and controls gene expression. It is required for binding of RNA polymerase to initiate transcription.
Recombinant DNA—
DNA produced by joining fragments of DNA from different sources by in vitro manipulations.
Replication-competent Virus—
A virus that can complete an entire replication cycle without a need for a helper virus; an autonomously replicating virus.
Restriction Endonuclease—
An endonuclease that recognizes a specific sequence of bases within double-stranded DNA.
Retrovirus—
A virus that contains reverse transcriptase, which converts viral RNA into DNA that then integrates into the host cell in a form called a provirus.
Serum-Free—
Refers to cell growth medium that lacks a serum component.
S Phase—
Part of the cell cycle during which DNA replication occurs (Synthesis Phase).
Stem Cell—
Immortal cell that is capable of proliferating and differentiating into different types of specialized cells. Each major tissue system is thought to have its own putative stem cell.
Suspension Culture—
Cells capable of growth in suspension, not requiring substrate (attachment) on which to grow.
Transduction—
Transfer and expression of genetic material into a cell by means of a virus or phage vector.
Transfection—
Transfer of DNA into cells by physical means such as by calcium phosphate coprecipitation.
Transgene—
Refers to the foreign genetic material delivered as part of a vector construct.
Vector—
The agent (plasmid, virus, or liposome–protein or DNA–protein complex) used to introduce nucleic acid into a cell.
Viability—
State of being alive and functional.
Virion—
An elementary viral particle consisting of genetic material (nucleocapsid) and a protein covering.
Virus—
Submicroscopic infectious agent that contains genetic information necessary for reproduction. It is an obligate intracellular parasite.
Western Blot—
An electroblotting method in which proteins are transferred from a gel to a thin, rigid support (e.g., nitrocellulose membrane) and detected by binding radioactively labeled antibody or antibody coupled to an enzyme, allowing use of a precipitating chromogenic or chemiluminescent substrate.
Xenogeneic—
From a different species.
Auxiliary Information—
Please check for your question in the FAQs before contacting USP.