Platelets
» Platelets is the portion of blood that contains platelet cells. It is derived from human whole blood from which red blood cells and a portion of the plasma are removed by centrifugation, sedimentation, or apheresis. In the apheresis removal method, the red blood cells and plasma are automatically removed and returned directly to the donor. Platelets derived from whole blood must be prepared within 4 hours after collecting the whole blood from which it is derived, or within the time frame specified for the blood collecting, processing, and storage system used.
Platelets may be derived from whole blood collected in any approved anticoagulant solution (see USP monographs for anticoagulant solutions). Platelets prepared by apheresis must be collected using Anticoagulant Citrate Dextrose Solution A as the anticoagulant solution.
Platelets derived from whole blood should have a minimum of 5.5 × 1010 platelet cells suspended in a volume of 40 to 70 mL of original plasma. Platelets produced by apheresis should have a minimum of 3.0 × 1011 platelet cells, suspended in 100 to 500 mL of original plasma or in an approved additive solution.
Platelets derived from whole blood or by apheresis may be further processed by filtration for removal of leukocytes, or by irradiation to inactivate lymphocytes. Platelets derived from whole blood may be pooled from multiple donors to form one dose of platelets.
Leukocytes may be removed from platelets by filtration, using an approved platelet leukoreduction filter. Platelets derived from whole blood must contain less than 8.3 × 105 leukocytes after filtration.
The source blood for platelets must be tested for syphilis, hepatitis B, and human T-cell Lymphotropic Virus (HTLV) Type I and Type II, using FDA-approved and -licensed commercially available test kits. The test results must be below the limits of detection specified by the manufacturers of the respective test kits. The source blood must also be tested for hepatitis C and HIV Type 1 and Type 2, using FDA-approved nucleic acid assays. The test results must be below the approved limits of detection for the tests used.
Packaging and storage—
Store platelets in an approved container. Platelets may be stored in plasma or in an approved additive solution at 20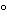 to 24
to 24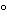 with continuous gentle agitation for no more than 5 days after date of preparation.
with continuous gentle agitation for no more than 5 days after date of preparation.
Labeling—
Label the container to indicate the collection date, the donation number or other coding means to uniquely identify the unit and to provide traceability to the donor, approximate volume, storage temperature, and its expiration date. Indicate the anticoagulant solution used and any additive solutions added subsequent to collection. Also label the container to identify donor status (for example, volunteer or paid). Label it also with the following statements: “See Circular of Information for the Use of Human Blood and Blood Components for indications, contraindications, cautions, and methods of infusion”; “Properly identify intended recipient”; “This product may transmit infectious agents”; and “Rx only.” In addition, label the container to indicate the product name as indicated in Table 1. [note—The name is determined by the method of platelets preparation (derived from whole blood or by apheresis) and by performing the necessary testing to ensure that the product meets the minimum requirements for the named products, as indicated in Table 1.]
[note—Platelets prepared by apheresis should be labeled with the donor's ABO blood group and Rh factors. Test the donor's whole blood or red blood cells as directed under Whole Blood or Red Blood Cells, respectively.]
Table 1. Names of Platelet Preparations
| Product Name | Method of Preparation |
| Platelets | Prepared from a single unit of whole human blood within 8 hours of collection. |
| Platelets, Pooled | Individual platelet units derived from whole human blood and pooled by aseptic techniques. [note—Label this preparation with a unique identifying number related to the number of individual units pooled, and with an expiration date of 4 hours after pooling of the individual units.] |
| Platelets, Pheresis | Prepared by apheresis from a single donor. |
| Platelets, Leukocyte Reduced | Prepared from whole blood, either by centrifugation or by sedimentation, and filtered using an approved platelet leukoreduction filter to yield less than 8.3 × 105 white blood cells in the final container. |
| Platelets, Pheresis, Leukocyte Reduced | Contains less than 5 × 106 white blood cells, prepared by apheresis, with or without a filter. |
Identification—
Dilute a small volume of Platelets 1:1000 with 0.9% sodium chloride solution. Place a small drop of the diluted platelets onto the end of a clean glass microscope slide. Obtain a second clean glass microscope slide, and draw its edge across the drop of platelets so that capillary action spreads the drop across the first slide. Push the second slide in one smooth motion across the first slide to make a smear of platelets. Allow the smear to dry. Apply a liberal amount (1 to 2 mL) of Wright's stain to the platelet smear, and allow to stand for 2 minutes. Dip the slide in deionized water, and gently blot dry with absorbent paper. Examine the slide using a microscope at 100× with bright illumination. Platelets appear as anuclear round or oval shapes approximately 0.1 to 0.2 µm in diameter, with some fine purple granulation. The platelets may occasionally appear to have a purple center with clear cytoplasm at the periphery.
Platelet count—
Use a commercially available, validated hematology analyzer to determine platelet count. Proceed as directed in the instrument's operating manual.
Residual leukocyte count—
Place 100 µL of Platelets into a suitable test tube. Add 400 µL of 0.01% (w/v) crystal violet in 15% (v/v) acetic acid, and mix thoroughly. Fit a hemocytometer with a 50-µL counting volume and a bright background with a cover slip. Load the counting chamber with the mixture until the counting area is completely covered, but do not overfill. Cover the counting chamber with a suitable moist lid to prevent evaporation, and allow to settle undisturbed for 10 to 15 minutes. Remove the lid, and place the chamber on the stage of a light microscope fitted with a 10× ocular lens and 20× objective. Count the leukocytes in the entire 50-µL counting volume. Calculate the leukocyte count in the platelets, expressed in leukocytes per µL, by dividing the observed leukocyte count by 10. Calculate the total number of leukocytes in the red blood cell unit as follows:
Total leukocytes = leukocytes/µL × 103 × volume of the platelet unit in mL.
pH 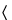 791
791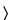 (for stored Platelets)—
Transfer aseptically a volume appropriate for the equipment: pH must be greater than 6.2 throughout the storage period.
(for stored Platelets)—
Transfer aseptically a volume appropriate for the equipment: pH must be greater than 6.2 throughout the storage period.
Auxiliary Information—
Please check for your question in the FAQs before contacting USP.
| Topic/Question | Contact | Expert Committee |
| Monograph | Anita Y. Szajek, Ph.D.
Senior Scientist 1-301-816-8325 |
(BBBBP05) Biologics and Biotechnology - Blood and Blood Products |
USP32–NF27 Page 1700
Pharmacopeial Forum: Volume No. 30(1) Page 166