Add the following:
INTRODUCTION
Proper microbiological sampling of microbiologically susceptible nonsterile products can be difficult because these products are often filled into unique primary containers that are designed to protect the product from inadvertent contamination during storage and use. These unique designs may increase the difficulty of taking an aseptic sample of sufficient size or volume for microbiological testing. Unless special approaches are used, products such as inhaled, nasal liquid, or powder dosage forms can be difficult to sample without potential exposure to extraneous microbial contamination. This general test chapter provides these special approaches for sampling either low- or high-content inhaled or nasal dosage forms. Alternative sampling approaches may provide better ways to sample containers in an aseptic manner. Any alternative methodology should employ aseptic techniques and should be conducted under environmental and other conditions that are appropriate for aseptic sampling.
INHALED OR NASAL DOSAGE FORMS
Low-content inhaled and nasal drug products (low-content INDP) are products that have a target fill of less than 100 mg of powder or 1 mL of liquid formulation per unit (primary container). Examples are pre-metered inhalation powders, more commonly known as dry powder inhalers (DPIs), and single-dose nasal sprays.
High-content INDP are multidose drug products that have a target fill of more than 100 mg of powder or more than 1 mL of liquid formulation per unit. Examples are aerosols for inhalation and nasal delivery, known as metered-dose inhalers (MDIs); device-metered inhalation powders; and multidose nasal sprays.
The appropriate sample quantity or volume should be based on the test methodology, including any relevant general test chapters, such as  61
61 Microbiological Examination of Nonsterile Products: Microbial Enumeration Tests and
Microbiological Examination of Nonsterile Products: Microbial Enumeration Tests and  62
62 Microbiological Examination of Nonsterile Products: Tests for Specified Microorganisms. Testing may be performed on the unpackaged bulk dry powder or liquid formulation or the finished product. If testing is performed on the bulk material alone, then the process leading from the bulk to the finished product should be validated for its ability to prevent microbial contamination. Testing should be performed on the finished product if this process is not validated.
Microbiological Examination of Nonsterile Products: Tests for Specified Microorganisms. Testing may be performed on the unpackaged bulk dry powder or liquid formulation or the finished product. If testing is performed on the bulk material alone, then the process leading from the bulk to the finished product should be validated for its ability to prevent microbial contamination. Testing should be performed on the finished product if this process is not validated.
SAMPLE SIZE DETERMINATION
For each microbiological test, sample 10 drug product containers or units or a number of units that can provide a minimum of 1 gram of product that are representative of the batch. For batch sizes smaller than 200 units (e.g., batches used in clinical trials), sample size may be reduced to 1% of the units or 1 unit, whichever is greater. The contents of individual containers may be pooled for testing.
BULK TESTING FOR LOW-CONTENT INDP
Bulk lot testing may be preferable for low-content INDP in lieu of finished product testing to allow larger sample sizes that are representative of the batch, without unduly increasing the risk of inadvertent microbial contamination. Bulk testing can be performed on the bulk powder or liquid formulation just before filling. If bulk testing is performed in lieu of finished product testing, then manufacturing processes following bulk sampling (e.g., filling and packaging) must be validated in accordance with current good manufacturing practice (CGMP) for their ability to prevent microbial contamination. For microbial enumeration tests, at least 10 g or 10 mL of bulk material, or, for specified microorganisms tests, 1 g or 1 mL of bulk material may be sampled. For small batch sizes (i.e., less than 1000 g or 1000 mL), the recommended sample size is 1% of the batch for both microbial enumeration and specified microorganisms tests.
SAMPLING METHODS FOR HIGH-CONTENT INDP
Dry Powder Inhalers
DPIs have an internal reservoir that contains a sufficient quantity of formulation for multiple doses that are metered by the device itself during activation by the patient. For DPIs, appropriate validated procedures should be used to sample a nonsterile drug product container.
Inhalation Aerosols
Consider safety issues related to both inhalation of the drug substance and the potential of a flammability hazard. Avoid contamination of samples by employing aseptic techniques whenever necessary.
automatic actuation method
The contents of the inhalation aerosol containers may be collected by automatically actuating each aerosol container and collecting the delivered formulation on a suitable sterile filter.
room temperature method
Disinfect the outside of the test containers with an appropriate disinfectant, and allow the containers to dry in a controlled environment. Empty the contents of the aerosol container into a sterile vessel using a needle apparatus or similar device (e.g., icemaker water line tap). If it has been demonstrated that the propellant does not inhibit the growth of microorganisms, the contents of the sterile vessel may be added directly to the liquid media or buffer for the test. Otherwise, allow the propellant to evaporate from the vessel by leaving the vessel at room temperature for several minutes. Remove any residual gaseous propellant by tilting the vessel slightly or by allowing a slow stream of microbiologically inert sterile gas to pass over the surface. For some less volatile propellants such as chlorofluorocarbon (CFC) 11/12 combinations, the vessel may be heated slightly (to temperatures 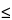 45
45 ) to assist with evaporation. After the propellant has evaporated, add the liquid media or buffer, and mix the contents to prepare for testing.
) to assist with evaporation. After the propellant has evaporated, add the liquid media or buffer, and mix the contents to prepare for testing.
Direct expulsion into the broth media or buffer may be feasible if a needle apparatus that is thin and strong enough to puncture the container and to allow slow removal of the contents is available. In this case, the contents may be expelled into and mixed with the aqueous medium. Layering of the propellant and aqueous medium may occur, in which case a longer time period and slight heating (not to exceed 45 ) may be required for propellant evaporation.
) may be required for propellant evaporation.
chilling method
Place the disinfected aerosol containers in dry ice, or a dry ice slurry (ensure the microbial quality of the dry ice and slurry-forming liquid), or a cryofreezer for the period required to liquefy the contents. Disinfect the outside of the test containers with an appropriate disinfectant, and allow the containers to dry in an aseptic environment. Aseptically open the aerosol containers using an appropriate tool. Be aware that freezing can affect the viability of microorganisms. For CFC-based products, pour the contents of the containers into sterile vessels. Allow the propellant to escape, and combine residues with a diluent appropriate for the drug product. Other drug-specific procedures may also be employed. For hydrofluoroalkane-based products, pour the contents of the containers into sterile vessels partially immersed in larger vessels containing dry ice. Drive off the propellant, for example by allowing a slow stream of sterile, filtered, oil-free compressed air to evaporate the material to dryness. Combine residues with a diluent appropriate for the drug product. An alternative procedure when testing the entire contents of a previously chilled container is to pour the contents of the opened container onto a sterile membrane filtration unit, allow the propellant to escape, and then rinse with an appropriate amount of sterile diluent.
Multidose Nasal Sprays
Multidose nasal spray containers usually have a cap that is screwed on, crimped on, or forms a snap-fit. The container can be opened by unscrewing the cap, cutting the seal, or using a decrimping tool, taking care to avoid microbial contamination during the process. Following cap removal, traditional sampling methods as described in general test chapters such as  61
61 Microbiological Examination of Nonsterile Products: Microbial Enumeration Tests and
Microbiological Examination of Nonsterile Products: Microbial Enumeration Tests and  62
62 Microbiological Examination of Nonsterile Products: Tests for Specified Microorganisms are typically appropriate for use.
Microbiological Examination of Nonsterile Products: Tests for Specified Microorganisms are typically appropriate for use. USP35
USP35
Auxiliary Information—
Please check for your question in the FAQs before contacting USP.
| Topic/Question | Contact | Expert Committee |
|---|---|---|
| General Chapter | Radhakrishna S Tirumalai, Ph.D.
Principal Scientific Liaison 1-301-816-8339 |
(GCM2010) General Chapters - Microbiology |
USP35–NF30 Page 253
Pharmacopeial Forum: Volume No. 36(6) Page 1667